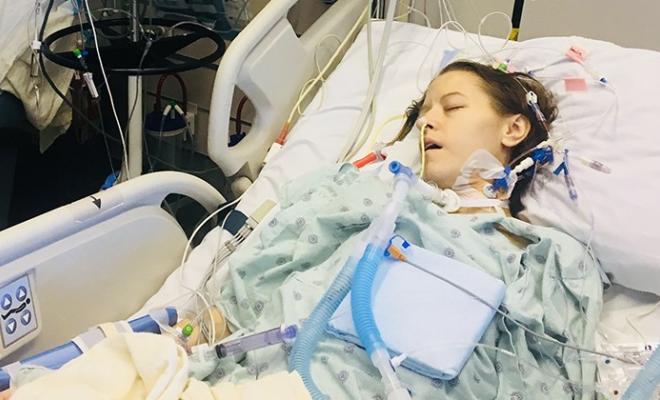
It will be 14 years ago this summer that I had my lung transplant. And these days, that 14 years feels like a lifetime ago. I can still remember the hours after the surgery, waking up and reaching for a telephone in the middle of the night, trying to call friends, trying to talk to someone, anyone. Not long after the surgery, I can remember my mother asking me how I felt. How I felt?
“I can breathe,” I said.
It wasn't for another decade that I realized how difficult it all was. Before the transplant, doctors and nurses told me how I'd be trading one disease, cystic fibrosis, for another -- lung transplantation. I'd nod politely. I told myself that I'd gladly cut off my arm if I could just catch my breath quickly after walking up a flight of stairs. So the idea of trading CF for anything else seemed trivial.
For me, the transplant itself was easy. I remember laughing to myself the night of the transplant. A lung transplant. It was cute, harmless. I realize now that I was probably in shock. It truly sunk in emotionally a few days later.
Past midnight, I shot up in bed awoken by a jolt of panic. I screamed and started clawing at my chest, trying to rip out the staples. My fingernails were bloody and I poured sweat. It was a panic attack. I was terrified.
The days, months and years after that were a mix of uncertainty, fear, hope, sadness and love. I finished college, started working and writing, and tried to move on with life. Life and death, CF, organ transplantation -- the struggle of it all was always in my head but buried deep down in some dark corner.
Wherever I went, people loved to remind me how lucky I was and how grateful I must be. And I was. All day, every day. But I never needed someone else to remind me of it.
To me, it was simple. I was born with a disease that I didn't want. I had a lung transplant because dying wasn't an option. I was happy to be alive. End of story.
But, of course, it wasn't the end. The emotional confusion and distress took a long time to understand. I began to travel. I started teaching in Europe and Latin America, running to and from nothing in particular, just trying to soak up as much life as I could. Eventually, I fell in love. I learned to laugh and cry and appreciate the details of everyday life. Years later, the transplant, CF and guilt all began to fade away.
For months at a time, I forgot that I was ever sick. No doctor appointments, no hospitals, no panic, no survivor's guilt, no disease, no CF, no transplant. It was like a heavy blanket of fog that lifted. It was this clarity that enabled me to truly reflect on everything that had happened. I wasn't afraid to sit with my thoughts anymore.
When I thought about the transplant process, I began to realize how emotionally harrowing it had been. Memories flooded back: Signing a living will at 19 and leaving my only possession -- a CD collection -- to my younger brother; thinking that I didn't want my older sister, who has CF, to go through all of this too; feeling that it would be better for everyone else if I pushed them away before the transplant in case I didn't make it; not talking to my parents and feeling so selfish and sad to not let them in; being angry, looking for some god to make the pain go away.
It was all of these things that hurt -- not the surgery or rehabilitation. It was the fact that I was 20 years old, scared and thinking the transplant would magically make everything ok. This idea of mental health was the truest, most difficult and constant struggle throughout the decades. And it's my biggest problem with CF. It steals your identity, creeps under your skin, digs in and doesn't let go.
I've known this for quite some time and, today, things are different. I approach CF with understanding and respect. Now, all of those moments are shadows of a memory. Passive and empty.
Today, I breathe in … I breathe out … I move on.