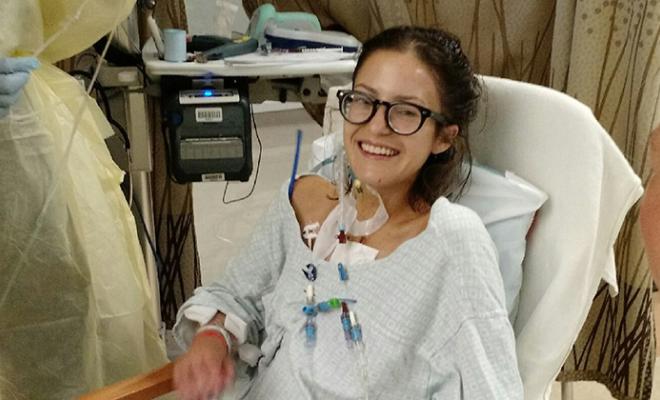
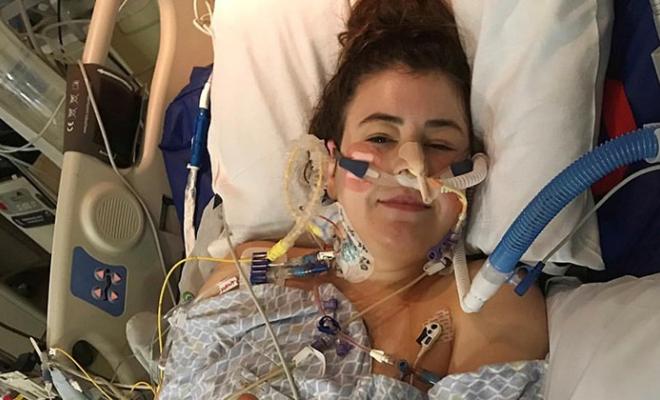
After a long struggle to become healthy enough to be considered eligible for a double-lung transplant, I spent the next 18 months — day and night — glued to my phone, full of the anxiety of missing my call for transplant. I slept with my phone by my head and the volume turned all the way up. I left my phone face up when I was away from home. Even in movie theaters, where I had to turn my volume all the way down, I would leave it in the cup holder to ensure I would see it light up if a call came through. I also avoided all areas without service and stayed within 4 hours of the hospital at all times (one of the rules while listed).
At 1:40 a.m. on Oct. 20, 2015, I was awoken as my mom crashed through my bedroom door. Stanford's heart and lung-heart transplant team had found donor lungs. The words “we have a donor for you” still echo in my head when I remember it. I immediately called my brother who expressed shock and disbelief. I must have texted more than 100 people on the way into the hospital to share the news and thank them for their support.
Within 30 minutes, we were at Stanford. I was overwhelmed when everyone greeted me with happy intensity. A room had been prepared for me on the general medicine floor where cystic fibrosis patients are usually hospitalized. A nurse checked me in and for the first time, we didn't review my medications. That was when it hit me. There was no need to review my current medications because they would soon be different, treating my new lungs and body instead of my past self.
Signing my consent for surgery was surreal. It felt like my future was full of possibilities and I never had to live day by day again.
After I checked in, my team began to prepare me for surgery, mentally and physically. The first to greet me was a fellow from my familiar transplant team to reassure me everything was as planned and wish me luck. For the next few hours I sat in the room with my mother, brother and friend while my transplant surgeon's fellow came in to go over the details of the surgery, have me sign many different consent forms, sign to donate my old lungs to scientific research, and familiarize us with who he was. Around 9 a.m., I was taken to the operating room (OR), my family walking with me, holding my hand and pumping me up with encouragement.
I felt strangely calm and reassured. I kissed everyone goodbye and realized that if something went wrong, this would be the last time I saw them. I squeezed extra tight, told each person I loved them unconditionally and was wheeled into the biggest OR I had ever seen.
There were machines everywhere and more team members than I had ever experienced before. There were nurses and technicians everywhere. Each had his or her own responsibility. Unlike the usual attitude of quiet competence that I found in most nurses, techs and surgeons, I sensed a feeling of fierceness in each team member.
I was instructed to lay on the T-shaped board that I would be on during surgery. Someone strapped me to the table for safety and placed heart monitors and an oximeter on me. The next step was accessing my port, securing an arterial blood gas line in my left wrist and placing a triple lumen line on the right side of my neck. Someone offered to give me some medication to soothe my nerves as the prep for surgery would take a little over two hours, but I refused. I wanted to be able to get confirmation the lungs were healthy and the surgery was going to take place before being sedated.
During more than two hours of preparation, the team received phone updates about the donor lungs. The donor team informed us that the lungs appeared healthy. They called again with test results for any “high-risk” possibilities such as cancer, HIV and sexually transmitted and other infections. The lungs were “perfect,” and the donor team was headed back with them. It felt real at that point!
An hour later (may I add that it felt like the longest hour of my life), my transplant surgeon called to tell us he was on his way into surgery. Thirty minutes after that, he walked through the door, completely excited and confident that the lungs were ready to be transplanted. At this point, I wrote a quick note for the surgeon to take to my family when he went to confirm that my surgery was a go. It reads, “I love you all with all my heart! I wouldn't be me without all of you. You're my world. Thinking of all of you!” It hangs on the refrigerator today to remind us of the moments we fought through as a family and that love conquers all.
All the people in this photo keep me motivated. They make me fight harder and love deeper, all through example.
To read Part 2, Unexpect the Expected: What I Learned After My Lung Transplant, click here.