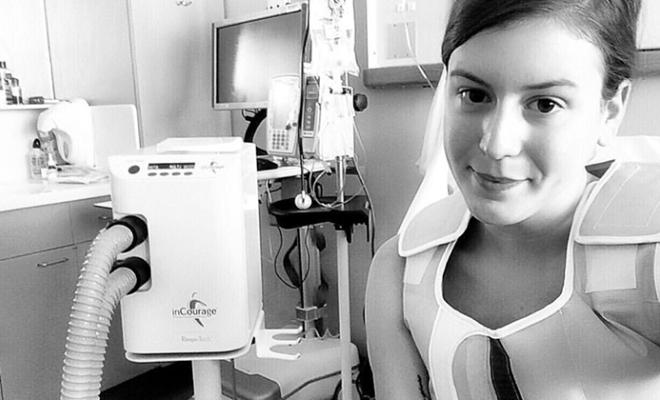
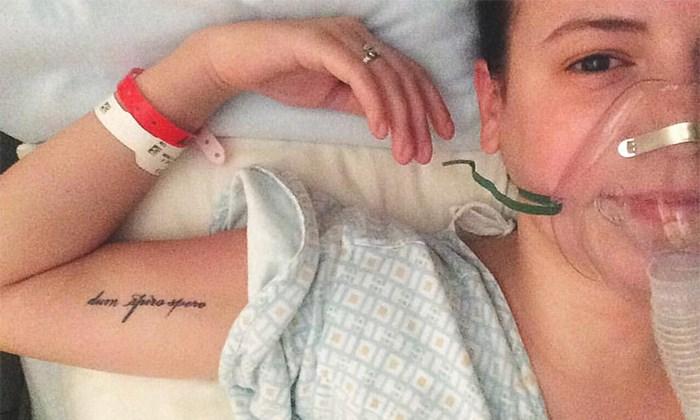
When I was diagnosed with cystic fibrosis at 4 months old, my pulmonologist said to my parents, “There will be a lot of different bacteria your daughter will culture, but the one we hope to never see is Burkholderia cepacia.”
You could say that the first 18 years of my life were “normal,” or as normal a life that anyone with a chronic lung disease can have. It wasn't until I was in the car with my mom and my sister on our way to Destin, Fla., for spring break that we received the phone call from my nurse coordinator saying that the sputum culture had come back positive for the bacteria.
I had never heard of this “bug” until I realized that I was now the proud new owner of it. B. cepacia are virulent bacteria found naturally in the environment, wet soil, decaying plants, and even the skins of onions, and is dangerous for someone with CF. The reason I had never heard of B. cepacia before was because only 3 percent of people with CF get it.
After my mom had finished talking with my nurse coordinator and told me the news, I started crying. “I knew it,” I said. “I could feel that's what it was while you were on the phone.” Since I was already on intravenous (IV) antibiotics, my doctor said that I didn't need to come in right away.
Once we were back from our trip, we talked about the next course of action. I had more than 19 hours to process what this meant for me, for my family, and for my future. I didn't realize it then, but my life was completely changed whether I was ready or not.
This is when I went into the Google black hole and started researching B. cepacia. I read articles in medical journals about how it was resistant to multiple antibiotics, statistics on how B. cepacia affects post-transplant survival, and how it could turn deadly if left untreated.
At 18, I was preparing to go away to college; I wasn't ready for this new complication of my disease. The same questions and thoughts kept swirling in my head. “Will I be able to go away to college?” “Will I now die sooner because of this complication?” These are thoughts no 18-year-old should have to face.
Luckily, my health stabilized, and I was able to go away to college and live the life of a college student. It wasn't until my sophomore year, toward the end of the first semester, that my health took a turn and I had to withdraw and move home. I was devastated. Moving back home and not being able to finish my undergraduate degree was a blow that took me several years to overcome.
Over the next several years, my health steadily declined. My lung function had gone from a forced expiratory volume (FEV1) of 60 percent to 40 percent. My health began to require hospital stays every 2-3 months, with weeks of IV antibiotics. I slowly started to become aware that my life could be coming closer and closer to the finish line.
This is when I made the decision to move halfway across the country to the Bay Area to focus on my medical care. It was scary to leave behind everything I knew, but also thrilling in the sense that I felt hope for a better quality of life.
It's been three years since moving to the Bay Area, and I thank God, karma, and the universe for giving me this extra lifeline each day. I am fortunate that right now, my health is stable; but with CF, things are always uncertain.
I still get those swirling thoughts in my mind of whether I'll ever be able to finish my degree, live on my own and be independent, get married, and have a family of my own. I also wonder whether my lungs will soon no longer be able to give me breath and I will need to have a lung transplant. I don't think those feelings and thoughts will ever cease, but this is the life I have, and I intend to live it.