My answer to that question is a complicated yes. And, in my experience, only up to a point. You can only balance two balls for so long until -- eventually -- one of them falls.
That's the relationship I have trying to balance my career and cystic fibrosis. Sure, there have been times when I've completely rocked this balancing act for years at a time, but eventually something gives, and I lose that sweet feeling of control that has helped me cope with this illness.
I've always been a go-getter. Someone who feels the need to prove herself -- not necessarily to others, but to myself. When you've been told at various points in your life that your time here is borrowed and going to college, having a career, getting married, having children, and leading what most would consider a normal life is not in the cards for you, you either believe what they say, or you decide to prove them wrong. I felt that by pursuing a career, I could demonstrate that I am strong, I am not worthless, I have purpose here, and this thing called CF does not define me. I have the control!
But, I also enjoy working because I thrive on schedules. It's a tangible way for me to see that I'm doing something with my life. Sticking to a schedule may also be why I excel at taking all my medications, doing my therapies, and making my doctor appointments. The schedule keeps me on point and has allowed me to balance the demands of a full-time career and a full-time illness, along with all the other things life throws at you daily.
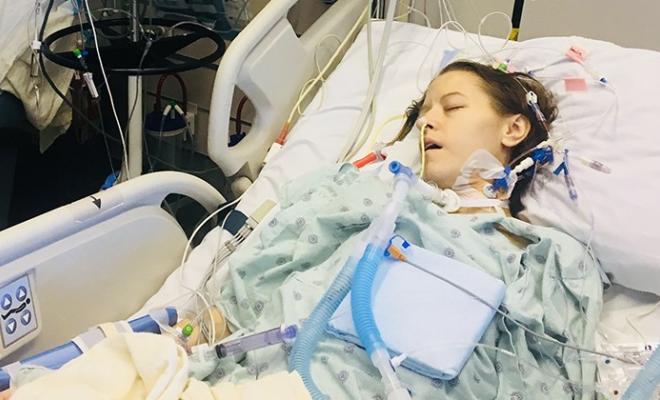
My lips were purple
This defense mechanism of overachieving despite my CF got me through some really difficult times; but when I look back, I realize that it was also the reason why I had those difficult times. I would push myself to the limit until I just couldn't go anymore and either needed to be hospitalized or had to cut something out of my schedule, or both.
The prospect of calling in sick always made me feel like I was weak. I was terrified of letting people down, and I felt like a quitter. I remember one night when I was working as a waitress, my boss made me leave because my lips were purple, and I was having a noticeably hard time breathing. Being sent home was a slap in the face because I knew I could no longer cover up my symptoms. I felt defeated that I had no say in the matter; yet it all became very real at that moment. Was serving food to strangers that important to me? Why did it take someone else saying it to make me realize something was really wrong here? Did my boss care more about my health than I did, or was I just trying to avoid what was really going on?
I neglected that fine balance I was trying to maintain, and my health suffered. I wish I could tell you that was the last time a boss made me go home because I was noticeably struggling. It's apparent now that I lack the willpower to say no when it comes to work because that feeling of accomplishment I get in return clouds my judgment. For me, the hardest part about having an illness like CF is that it always finds a way to prove me wrong, to make me stop, to make me finally cave and say, “Fine! You win!” The loss of control is what torments me, yet it drives me to keep striving for more.
Was it worth it?
About six years ago my CF “won” in a big way. My lungs just couldn't take it anymore, and I thankfully received a double-lung transplant. My recovery went very well, and for once in my life, I felt healthy. This renewed sense of well-being, coupled with my determination to help others, led me to a career as a probation officer.
I had so much energy and was getting more done in a day than I'd ever imagined. I was waking up at 5 a.m., going to the gym, going to work early and staying late, entering climbing competitions (and winning), filling my weekends with adventure, and getting a good night's sleep. The juggling act was in perfect motion. And, to top it all off, I wasn't canceling, missing, or rescheduling anything. I was actually accumulating sick leave! This precious piece of evidence is what fueled my eagerness and reassured me that I was doing something I could be proud of.
When I finally felt like I needed a change, I transferred to another department and finally found my niche as an alternative sentencing case manager. About a year and a half later, my lungs began going through chronic rejection. In what felt like a split second, I was ripped from this dream job into a life supported by ventilators, feeding tubes, and IV treatments. All the control I had gained, my perfect balancing act, toppled.
I was grateful that I had accumulated so much sick leave, comp time, and vacation time, but within three months I had exhausted it all in the hospital waiting for new lungs. There were times that all I could think about was, “Why didn't you use that vacation and comp time to go somewhere you'd never been?”
Did I work myself so hard in the last five years that what I brushed off as healthy stress actually wasn't? What is all this hard work for when you're too sick to reap the rewards? Was it -- and is it -- worth it?
After three months of this constant back and forth in my head everything went silent. I welcomed the silence as it's hard to think about your future when it relies solely on the end of another's.
I need to take care of myself
I think I'll always have that internal struggle and dialog with myself. Is working doing more harm than good? Would I be healthier if all I had to do all day was focus on my health regime? It may be safe to say there's a good chance I'd be more physically healthy but at what cost toward my mental health? No one can answer these questions for me, but it puts my mind at ease that I've grown up enough to be able to ask them. Since my second double-lung transplant, I have had more ups and downs. Despite telling myself in the hospital that I wouldn't take work so seriously anymore, I found myself asking my doctors three months post-transplant when I could go back to work.
Just a year after this health crisis, I'm back at my job -- only now I work 28 to 32 hours a week. My coworkers, supervisor, and boss are amazing. They are better than me at making sure I'm out of the office after a certain time and support me no matter what decision I make -- or should I say, my illness makes for me.
As I'm writing this blog I am attached to an IV pole with the hope of reducing the size of an abscess that has collected in my throat. The biggest challenge I face is not letting the stress of missing work stress me out more. Even though I'm 37 and have been through so much uncertainty with my health, I still haven't learned how not to be so hard on myself.
This overwhelming need to not let CF dictate my life is a way to mask what I'm afraid of realizing: That I do get sick. I do need rest. I need other people to help me, but I also need to take care of myself.
Because when it's all said and done, I want to feel as though I have gotten something out of my life. I want the balancing act to be worth it.