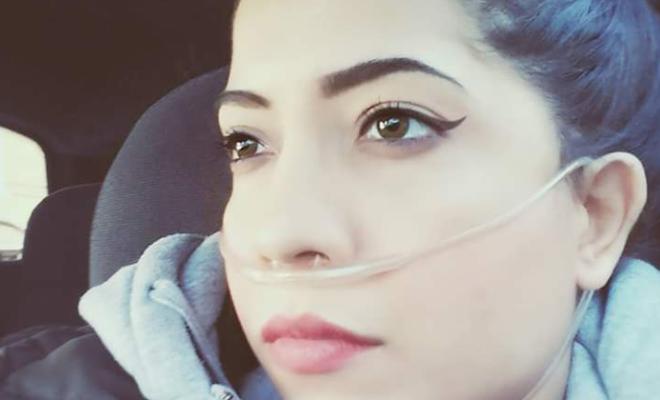
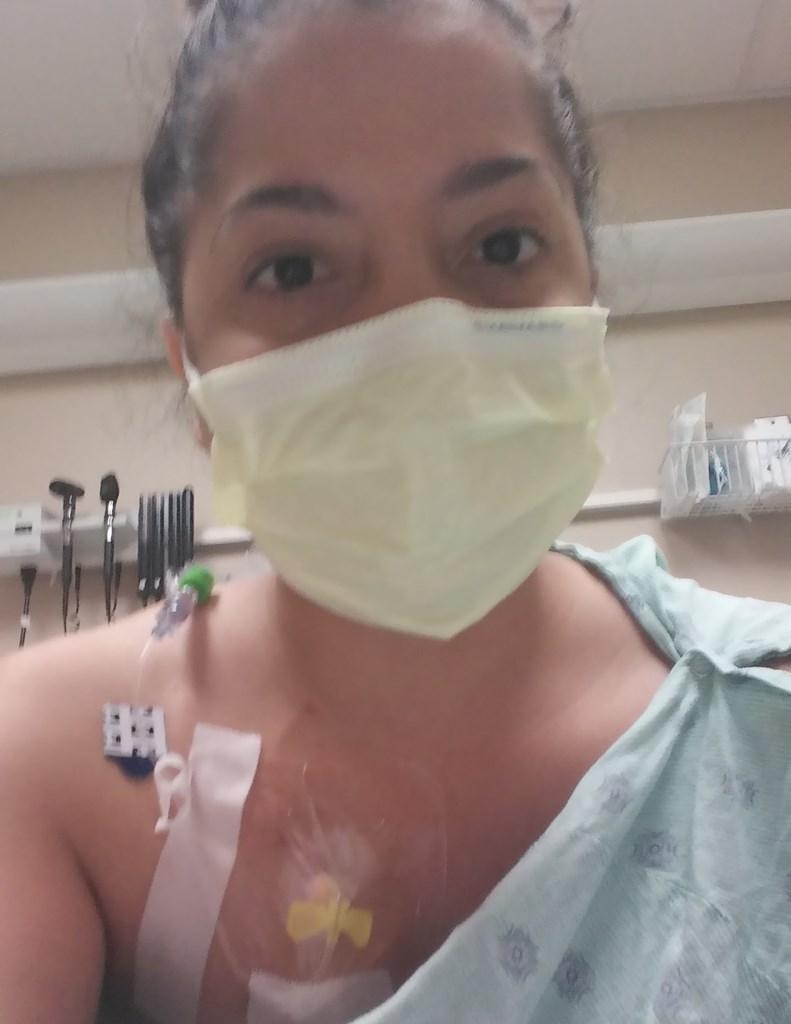
Having CF is painful, at least for me it is. For as long as I can remember, pain has been a daily occurrence, but I've learned to live with it. When I was a teenager and first began fully experiencing pain that could not be relieved with over-the-counter pain medications, I was prescribed a stronger pain reliever.
I felt good! Being pain-free was so intoxicating (no pun intended). I no longer felt pain from moving, coughing, or breathing. I didn't expect for the medication to drown out my mind, but it did, and it felt good. I wasn't thinking about dying anymore. I was fine for the first time in a long time and I liked that feeling.
Soon, I was taking the medication more often than I was supposed to because, eventually, I needed more of it to continue feeling “normal.” I couldn't think about anything else because of how the medication affected my mind. I no longer had a ticking clock in my head, constantly reminding me that I will expire sooner than everyone I knew.
I was functionally “high.” No one knew what I was doing or could tell either. It surprised me how well I could hide what I was doing, how well I acted normally. How, when I needed my pain pill, I could take it without anyone thinking anything was wrong because it looked like I was taking an antibiotic or enzymes.
I became pretty good at hiding it. Years flew by like that. I just could not stop. I knew I had a problem, but I never really confronted it because I was ashamed that I had let myself get into that position. I was embarrassed and I did not feel like I could tell anyone. I was alone.
One day, I finally got the courage to speak to my doctor about it. He recommended that I wean off the medication slowly because I had become dependent on it. He told me, honestly, that withdrawal is not the best experience. But, I was stubborn and didn't listen. I went home and flushed the pills because I just wanted to be free. Within an hour, I began to experience withdrawal symptoms. I was sweating, vomiting, had horrific stomach cramps, and was restless. I was just miserable and I was like that for several days.
I lied to my family and said that I had a bad stomach virus. I was too ashamed to tell them anything, and I carried that shame for years before I told them the truth. When I finally did tell them, reality was the opposite from what I imagined. They supported me 100 percent. I was scared for nothing.
Having CF, and everything it comes with, means pain, that includes bronchiectasis, arthritis, joint pains, fibromyalgia, abdominal cramps, cracked ribs from coughing too much, medication side effects, and surgeries. The list is long, and -- like many other CFers -- pain is just a huge part of our lives.
I now have a high tolerance for pain. I monitor my pain medication, meaning I only take it when walking becomes agonizing or the pain is unbearable. I wear compression socks and I wrap my knees and ankles. I use pain patches and I soak my worn-out body when I have to. I have found other ways to cope and I'm happy with that progress because I'm not dependent on pain pills anymore.
I wanted to speak up about it now because I'm not ashamed or scared anymore. It was a long road to get to where I am, but I made it. Pain may still be a part of my life, but it doesn't own me anymore.
Join the conversation on Facebook.