As I have gotten older, the reality I have faced is that people with CF are performing a never-ending balancing act. Each misstep causes us to become more and more unstable until, one day, we tragically fall -- at the mercy of whatever lies below.
But what if we were told that a medication would come out that could change all of that? Rather than be at the mercy of gravity, we'd have a safety net no more than 3 feet below us. So, in the instance of falling, the rebound would be essentially a piece of cake. If you had told me this two years ago, not only would I have been in utter disbelief, but I probably would have laughed so hard that I would have had to spend the better part of my day coughing to recover.
But the reality of today is that we are on the precipice of a new frontier for cystic fibrosis -- a frontier in which children born with CF today have the potential to live very different lives than any from a previous generation.
Rather than spending hours upon hours a day doing breathing treatments in hopes of delaying the serious effects that some of us know all too well, today's children with CF might grow up learning to accept their diagnosis as part of their indefinite reality, rather than of their ultimate demise.
Upon the approval of Trikafta® last year, exhilaration buzzed throughout the entire medical community, making it sound like it was nothing short of a dream come true! Medical journals that I'd seldom seen talk about CF in the past were now frantically devouring the miraculous data from this new CFTR modulator that was more efficacious and available to more people with CF than any other CF treatment that came before it.
While the approval of Trikafta was undeniably special to everyone, the feeling it carried for me was likely similar to the smaller group of patients who initially qualified for Kalydeco®, since this was the first modulator to work for my “eclectic” combination of a relatively uncommon nonsense mutation and F508del.
My first dose of Trikafta gave me a feeling of unbreakable optimism for my new life to come. And while I'm not usually very spiritual, in this moment I felt the overwhelming need to express my gratitude to the higher powers of our world for this new drug, and for keeping me somewhat healthy so I could truly benefit.
Four days after I started Trikafta my lungs were already feeling great! I was waking up to a full and fresh breath of morning air, rather than a stale, choking sensation from forcefully coughing up thick, tar-like mucus out of my larger airways. At the same time, however, I started to notice something else was very wrong.
I hadn't been able to pass stool since before taking my first dose of Trikafta, which -- at this point -- was rapidly approaching five days and causing me a great deal of physical pain. I reached out to the on-call CF clinician and described to her my worsening symptoms. She concluded that if I didn't pass stool by the end of the day that I would likely need to be admitted to the hospital for a probable bowel blockage.
The news of this instantaneously shattered my newfound bubble of invincibility that I had built for myself no less than a few days prior. Like many of us, I couldn't help but fall back onto the worst thoughts that my brain could generate: Did I legitimately have a bowel blockage? Was it potentially life-threatening if left unresolved? Was this the end of my new relationship with Trikafta? Would this become a new, chronic manifestation of my disease going forward?
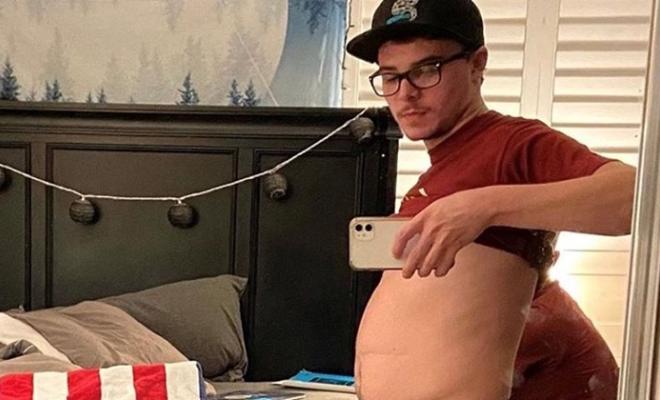
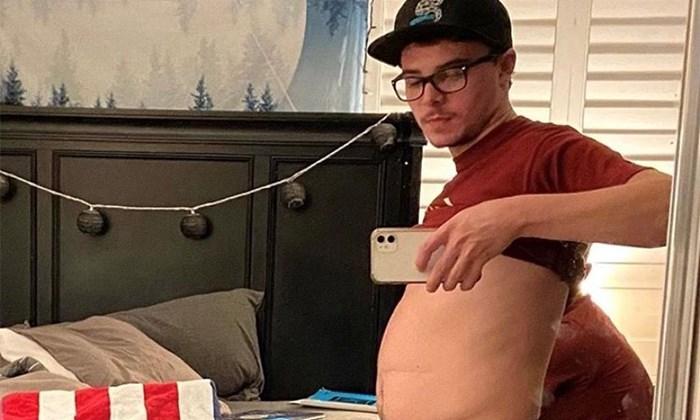
Aside from being born with a severe intestinal blockage common to infants with CF known as meconium ileus, I've never suffered such intestinal issues in my childhood and teen years. Alongside the inability to pass a proper bowel movement in the absence of daily laxatives, I've also developed a noticeably chronic bloat that has now prevented me from fitting into more than half of my go-to T-shirts, and arguably has been one the more challenging aspects in regards to my mental wellness surrounding the entire situation.
While high-dose laxatives thankfully returned my digestive tract to its prior state of function, my other fears were about to come true. Fast forward six months, and my lungs were still thriving! I had been off oral and IV antibiotics for almost a year. With the permission of my doctor, I was allowed to try reducing my dependency on airway clearance treatments from 60 minutes a day to about 30 (at times where my health permitted it, of course). However, the hurricane that is my digestive tract continued to spiral out of control. I was, and still am, dependent on daily Miralax clean-outs simply to function.
That being said, the difficulties of my GI circus actually haven't been the physical complications alone. It's also the comments and criticism from others, some of whom are also taking Trikafta, who have been fortunate enough not to experience such adverse events. All too often I'm met with responses such as, “your belly looks fine, calm down” or, “stop shaming yourself when you could just focus on better things.” Better yet, I've heard that “you're not grateful enough for what Trikafta has done,” and that “if you didn't eat as much as you used to, that maybe you'd put yourself out of your own consequential suffering.” I can see that some of these comments are innocent enough and come from the individual's naiveté about my personal circumstances, but it is anything but reassuring.
At the very root of my complex emotions about being on Trikafta is the emotional pain that comes from losing control over a part of my body that wasn't in jeopardy before.
So, while I am eternally grateful for benefitting from modern medicine, I shouldn't have to apologize for being upfront about the pros and cons of my experience with Trikafta. Putting my own experiences aside though, the fact that only close to 90 percent of people living and fighting with CF every day have access to an effective protein modulator is unacceptable. While it may not be of the greatest importance to those that already have access, it is vital that we do all in our power to fight the loss of more and more invaluable lives to this beast of a disease.
Additionally, for people like me who have no choice but to grapple with a love/hate relationship to Trikafta, there needs to be a broader variety in treatment options. So many don't qualify for any of the previously approved modulator drugs. Further innovation is more important than ever even in the age of significant progress for most. There are still many people anxiously anticipating their miracle pill, not to mention those in need of one better suited to their individual needs with CF; we are all different regardless of our shared diagnosis! Until that day comes, I will continue to fight the good fight for me and everyone else out there still kicking CF's butt like never before, until CF stands for Cure Found, you all have my word!
Interested in sharing your story? The CF Community Blog wants to hear from you.