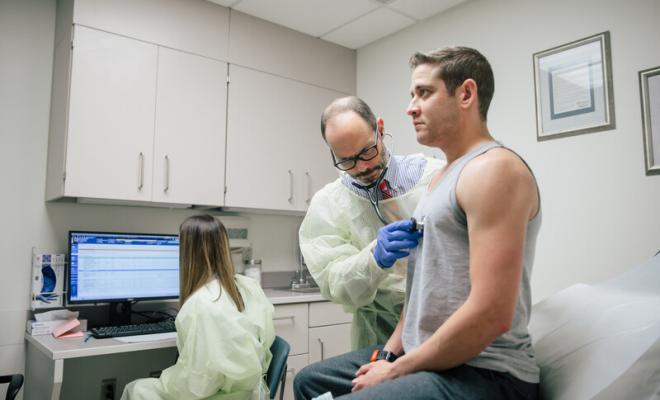
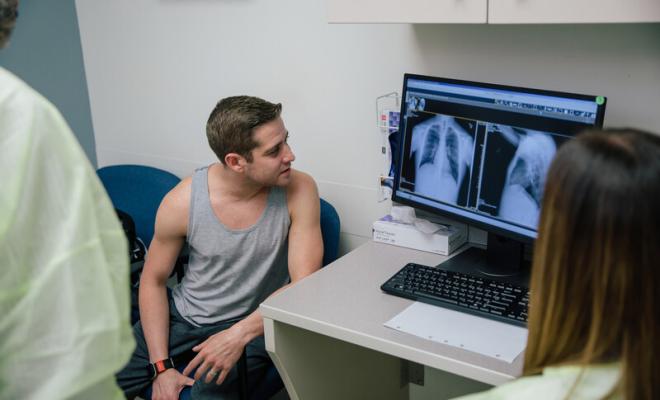
An early referral allows you to meet with the transplant team before moving forward with an evaluation for a lung transplant. Other times, the transplant team may recommend completing part or all of the transplant evaluation after your first visit. Referral is not the same as an evaluation, and an evaluation does not necessarily lead to listing for transplant. The goal is to identify any potential barriers to listing and attempt to address them prior to your need for listing for a transplant.
Although declining lung function is important to help your cystic fibrosis care team determine if they should refer you, there are additional factors that your care team will consider before they recommend that you meet with a transplant team and possibly be evaluated for a lung transplant.
Lung Function
Although it's not the only factor, declining lung function is a key indicator for transplant referral. Cystic Fibrosis Foundation lung transplant referral guidelines recommend that your care team talk to you about lung transplant as a possibility when your forced expiratory volume in one second (FEV1) drops below 50 percent predicted. The guidelines recommend that care teams recommend referral for transplant when FEV1 is less than 50% and lung function has declined by more than 20% in 12 months.
Most people will not need to receive a transplant at this stage, but it is important to start the conversation early.
Talking about transplant early will give you more time to work with your CF care team to learn as much about the transplant process as possible, including the benefits and risks, and to identify any factors that may prevent you from being listed.
Overcoming barriers to being listed could take time, so the sooner they are identified, the more time you, your family, and your CF care team can have to work on them. Additionally, talking about transplant prior to you needing an urgent evaluation or listing gives you the opportunity to make a fully informed decision without the added pressure of being severely ill.
| When | Your care team may |
| 1. Your FEV1 is less than 50% | Talk to you about transplant as a possible future option |
| 2. Your FEV1 decreases to less than 40% without exacerbation |
|
| 3. Your FEV1 decreases to less than 30% predicted without exacerbation | Refer you for transplant evaluation |
Markers of Increased Disease Severity
Although declining lung function is an important measure, other factors have been identified that may signal the need for referral — even if your lung function is not low enough to qualify for immediate transplant. Care teams may consider these factors in addition to lung function, or independent of lung function, when deciding when to recommend transplant referral. These factors are referred to as “markers of increased disease severity,” and include:
- Inability to walk 400 meters (about 440 yards) in six minutes (called a six-minute walk test).
- Hypoxemia.
- Hypercapnia.
- Pulmonary hypertension.
- When your body mass index (BMI) is less than 18.
- When you have more frequent pulmonary exacerbations — more than two pulmonary exacerbations per year that need to be treated with intravenous (IV) antibiotics or one exacerbation that requires positive pressure ventilation using bilevel noninvasive ventilation or mechanical ventilation via tracheostomy or endotracheal tube.
- Massive hemoptysis.
Because these markers may indicate shortened survival, the guidelines recommend that people with severely reduced lung function (FEV1 less than 40%) and one or more of these markers be referred for transplant. In addition, when lung function decreases to 40%, care teams may begin to look for markers of increased disease severity.
Other Circumstances
In addition to lung function and markers of increased disease severity, your care team may also recommend a lung transplant referral if:
- You are a woman between the ages of 18 to 25 years and have CF-related diabetes, rapidly declining FEV1, or rapidly declining BMI.
- You are less than 5 feet 3 inches and your FEV1 is less than 40% of predicted.
- Your BMI is less than 18 and your FEV1 is less than 40% of predicted while you are trying to gain weight.
- Your FEV1 is less than 40% of predicted and you have more than two pulmonary exacerbations per year that require IV antibiotics.
- You have one pulmonary exacerbation that requires positive pressure ventilation, in which case your care team may recommend a transplant referral despite a higher FEV1.
- Your FEV1 is less than 40% of predicted and you have massive hemoptysis that requires admission to the intensive care unit (ICU) or bronchial artery embolization to stop the bleeding.
- Your FEV1 is less than 40% of predicted and you have had a pneumothorax.
Emotional Support
The process of waiting for, receiving, and then recovering from a lung transplant can be long and stressful — not just for you, but also for your loved ones. You and your family may want to talk to others who are going through — or have gone through — a lung transplant to understand what you're feeling — both before and after the transplant.
"It is equally important for family caregivers to have ideas for keeping their loved ones' mental health intact. For example, my mother purchased a small fan for my room because my hot flashes made me feel miserable. She also asked the doctors if I could suck on hard candy since I was unable to eat or drink for weeks." — Jenavese Armstrong, an adult with CF, from the CF Community Blog
"I think there is some uniformity in the outpatient evaluation process. It's typically a 3 to 4 day process and I think the testing is very similar at different sites. What differs somewhat among programs is how early they want to see patients go through the evaluation process. Some transplant centers look at records and think they can predict well what the disease course is going to be and make a conclusion that it's too early [for transplant referral] and ask patients to be re-referred when their disease progresses. I generally am not a big fan of that approach, frankly, because I think we don't predict the future very well." — Joseph Pilewski, MD
You will need similar support after your transplant. Keep in mind that people with CF who have undergone a lung transplant still can get — and spread — dangerous germs among others with CF because these germs can remain in the upper respiratory system. Because of the risk of cross-infection, people with CF should take the same precautions they took before lung transplantation.
Make sure your transplant center has support groups or can help you find one that's appropriate for you to minimize the risk of cross-infection after your transplant. It is equally important to have family and friends nearby to support you in both good times and bad. You'll experience both as you navigate the transplant process.
There are aspects of transplant that people don't understand unless they have been through it themselves. CF Peer Connect is a one-to-one peer support program for people with CF and their family members ages 16 and older. Connecting with a peer mentor provides an opportunity to talk with and learn from someone who is also affected by CF and has gone through similar experiences, such as lung transplant.
Another form of social support from the CF community can be found in virtual conferences and events. Designed by and for adults with cystic fibrosis and their families, community conferences — including BreatheCon, CF FamilyCon, ResearchCon, and NextBreath — provide the opportunity to connect, share, and learn from peers through open and honest dialogue.
Institution-Provided Support
Your lung transplant center may offer you support throughout the transplant process, including psychological support, education, support groups, and Facebook groups. Some transplant centers have access to transplant psychiatrists, who are doctors trained in psychiatry with a special focus on individuals going through the transplant process. Learn about transplant centers across the country, including the one you may be referred to by your CF care team.
What Does It Take to Be a Candidate for Transplant?
The supply of donor lungs is limited and the transplant process requires a lot of work and commitment from you and those around you. That commitment, along with many other factors, can increase your chances of surviving the surgery and recovering afterward. The purpose of the evaluation is to help the transplant team determine if you would be likely to have a successful transplant.
A transplant team may determine that you are at too high a risk of doing poorly with the transplant surgery or after the surgery at their center. Factors that led to the decision to decline you for transplant at that center are referred to as barriers or contraindications to transplant. Depending on the specific barrier, there are some that you may be able to overcome.
Learning about these barriers as part of the early referral process for transplant can give you more time to work with your care team and to improve and become a stronger candidate for lung transplant.
"As I prepared to leave the hospital, I asked for a list of all the reasons I wasn't able to be listed for a transplant. Then, my team, my family, and I made the list of 'impossible' goals. I placed the list on the front of my refrigerator, my [do not resuscitate] form on the side of the fridge. Every day for that next year, I dedicated myself to checking items off that list until I was done." — Caleigh Haber, an adult with CF and two-time lung transplant recipient, from the CF Community Blog
Barriers That Are Harder to Change
Some of the barriers to transplant that are harder to change include:
- Certain infections (Burkholderia cenocepacia, Burkholderia gladioli, Burkholderia dolosa, Mycobacterium abscessus, and Scedosporium prolificans).
- Poor kidney function (called renal insufficiency).
- Liver disease.
- Critical or unstable clinical conditions, such as mechanical ventilation or extracorporeal membrane oxygenation (ECMO).
- Heart problems.
- Past chest surgery (e.g., surgical treatment for pneumothorax).
- Past lung transplant.
- Past cancer.
Although you may not be able to change any of these factors, many transplant centers have different policies about what they consider barriers to transplant.
Although some transplant centers may not accept people with certain health conditions, others may. For this reason, it is important that you understand the policies of a given transplant center and research more than one center.
The following organizations offer CF-specific information to help you learn more about lung transplant centers:
- The Scientific Registry of Transplant Recipients (SRTR) gathers a wide range of information on transplant waiting lists, donor-recipient matching, and transplant recipients in the United States.
- The International Society for Heart and Lung Transplantation (ISHLT) maintains an international transplant registry that contains statistics on outcomes, survival, and risk factors, which it updates yearly.
Barriers You May Be Able to Change
Barriers to transplant that you may have more control over include:
- Being underweight: If your body mass index (BMI) is less than 18, it may prevent you from being listed for a transplant. However, your care team can help you gain the necessary weight with nutritional supplements or placing a gastrostomy tube (G-tube).
- Substance misuse, including long-term use of opiates or narcotics, inhaled marijuana, alcohol, and inhaled tobacco products: Your care team can help you find treatment including behavioral treatment, medication, outpatient or inpatient treatment, and peer support.
- Cystic fibrosis-related diabetes (CFRD) that is not well-controlled: People who cannot manage their CFRD well are more likely to experience pulmonary exacerbations and have weight problems. In addition, the transplant team may see it as a lack of commitment on your part to sustaining your daily care.
Starting the conversation about lung transplant before you need to be listed gives you more time to work with your CF care team to address these potential barriers. Working to correct the identified barriers to transplant will show the transplant team that you are engaged in your care and that you want to become a stronger candidate for transplant at their center.
"I also feel it is extremely important for the CF care center team to advocate for their patients. You will see in my video how lucky I have been to have such a wonderful CF care team that worked to find a transplant facility." — Mindy Ladd, adult with CF, from the CF Community Blog