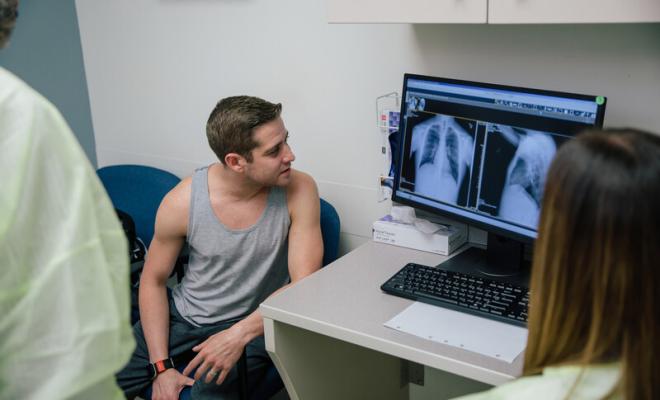
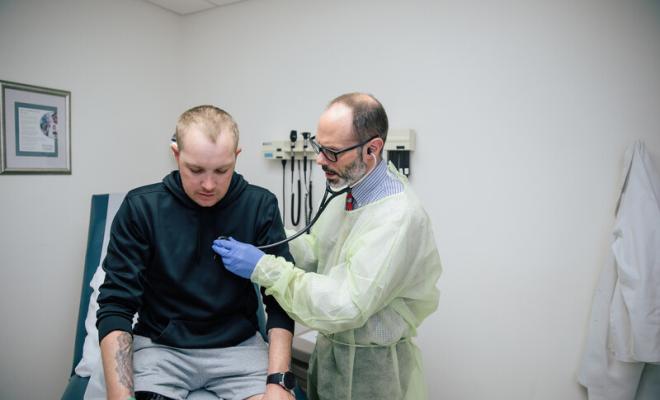
The evaluation process gives you the opportunity to learn more about a transplant from the transplant experts and to help you make a fully informed decision when determining if lung transplantation is right for you.
The transplant team will use the information gathered during the evaluation to determine if having a lung transplant is in your best interest during a transplant evaluation meeting. During this meeting, the transplant committee will determine that you will:
- Not be approved for a transplant because you have decided not to pursue transplant as a treatment option.
- Not be approved because you are too sick to undergo the surgery.
- Not be approved yet because additional testing needs to be done or barriers need to be corrected.
- Not be approved because you have factors that would lead the transplant team to conclude that transplant could be harmful to you.
- Be approved for listing.
If the transplant evaluation team concludes that you would be a successful candidate for a lung transplant, you will need to consider whether you are ready to be listed for transplant. After approval, you can be added to the United Network for Organ Sharing (UNOS) national waiting list to receive donor lungs. Whether your transplant team believes you would have a successful transplant may not be in your control, but you have the ability to make a fully informed decision about when you list if they do.
When the transplant team recommends listing, they are considering factors beyond how sick you are physically, such as the donor availability for your blood type and height, your antibody status, and any issues with your body that might make finding a donor more challenging. If you have concerns about the timing of listing, ask the transplant team and they may help resolve your questions. You may find that there are important factors that they are considering that are specific to transplant medicine.
https://www.instagram.com/p/BJvAuKOAzaf/
If you and your CF care team decide that you would like to be referred for a lung transplant, your care team will contact the transplant center and provide your medical records. You will then work with the transplant program to schedule an appointment.
The evaluation process involves many tests and consultations and may take up to several weeks. You will sometimes have to travel to the transplant center and stay nearby until the evaluation is complete.
Like your cystic fibrosis care team, there is a multidisciplinary transplant team. This team of health care professionals is highly trained to support the transplant candidate. During the evaluation, you will meet the members of this transplant team, which may include:
- Transplant surgeon
- Transplant pulmonologist
- Transplant nurse coordinators
- Social workers
- Physical therapists
- Respiratory therapists
- Dietitians
- Financial coordinators
During the evaluation process, the transplant team will review your physical health, psychological health, finances, and any potential factors that might prevent you from having a successful transplant to determine if you are eligible for a lung transplant.
It might feel uncomfortable to have certain aspects of your life and health examined by people you've only just met. But, the evaluation is essential to help the team members learn as much as possible about you so they can ensure that having a lung transplant will not be harmful to you.
At the end of the evaluation, the transplant team will meet to discuss your results and decide whether a lung transplant is appropriate.
Medical Evaluation
You will undergo testing that will help the doctors on the transplant team understand how well your body is functioning. The results of the tests will show how well your lungs, heart, and kidneys work. Other tests will be done to determine what kinds of germs you have in your lungs.
The results of these tests might require further testing, or they might determine that you would not be a good candidate for transplant at their center. Having an untreatable kidney disease is one example of something that might prevent you from moving forward in the transplant process at centers that will not consider multiple organ transplantation.
Psychological Evaluation
The transplant process is difficult, not only physically, but also emotionally. The transplant team needs to be sure that you will have the strength and support you need to cope with the challenges that you will face before, during, and after transplant.
For this part of the evaluation, you will meet with a social worker or a psychologist, who will gather information about you, your family, and your support system. Your ability to take medications every day as prescribed and abstain from smoking or illegal drug use will also be evaluated.
The psychological evaluation may result in the transplant team deciding that a transplant is not a good option for you. Having an inadequate support system is an example of something that might prevent you from doing well after a transplant and, therefore, prevent you from being put on the transplant list.
Financial Evaluation
You will meet with a financial coordinator, who will look at your finances, help you understand what your insurance company will cover, and help you plan for how you will pay for the expenses that are not covered. It is important to know that transplant candidates must show the financial coordinator that they can pay their share of the transplant costs and post-transplant care.
If the financial coordinator determines that you have insufficient financial resources to pay for your pre- and post-transplant needs, such as medication co-pays or relocation expenses — which are not often covered by insurance — you may not be recommended to move forward in the transplant process.
If the Transplant Team Recommends Listing
If your transplant team believes that you would have a successful transplant surgery, they will recommend that you be listed for a transplant. The transplant team will contact you when your name is added to the national lung transplant waiting list. Talk to the transplant nurse coordinator at your transplant center if you have any questions about your status on the waiting list.