A lot can happen in a year. Babies are born, people marry. A loved one can pass on. You can be happy and sad, frustrated, and glad. You can lose your mind a little bit and find yourself all over again. Life can seem cruel one day and the next like a remarkable gift. The disaster of 2020 was both inexplicably awful and quite literally breathtakingly beautiful for me. I fought my way out of a grave so deep that I still sometimes don't believe that what I am now able to feel is real.
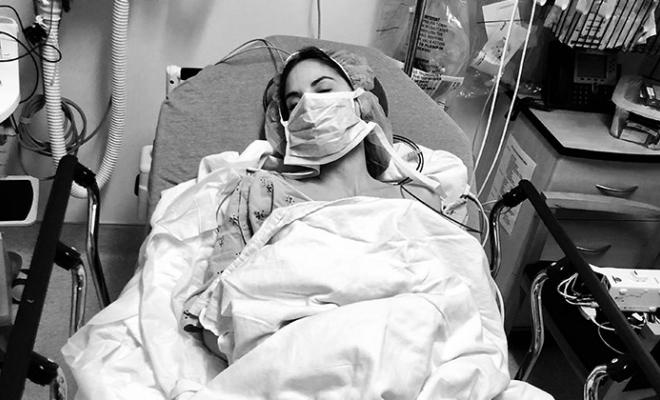
This time last year I was dying. Wearing supplemental oxygen every second of every day, I was dragging an oxygen tank around my house while still trying to function as a person, as well as my most cherished and important role -- a mom. In the span of a few months I had traversed from functioning sans oxygen to relying on it full time. My nine- and 12-year-old children watched as their mom declined more and more each day -- weak and struggling to breathe -- barely able to walk from room to room yet determined to fulfill the domestic duties I imposed upon myself.
I never wanted the reality and progressiveness of cystic fibrosis to halt the part of my life I loved and held tightly to, yet -- everywhere I went and looked -- I was reminded that I was now at a severe disadvantage.
My disease was front and center, making its messy presence felt in every single thing I did. Tubes tethered me to walls and machinery, and rows of pill bottles lined my counters and cluttered my mind.
Every day I fought a battle to survive, yet I was up against an opponent whose size and strength was daunting, destructive, and unrelenting, yet I refused to let my guard down and admit defeat. I knew I had to hold on and fight my hardest to reach my goal of a double lung transplant, which would be the hardest yet most rewarding adventure I'd ever dare to take. However, my life reached a crescendo that nothing could have prepared me for.
Like everyone else, I was blindsided when SARS-CoV-2, the virus that causes COVID-19, took down the world. I went into absolute isolation with my husband and children and -- for months -- we quarantined, not seeing a single other person, hoping and praying my call for a double-lung transplant would come sooner rather than later. By that time, I had been on the transplant waitlist for six months, and life was incredibly challenging. While I was suffering immensely, I still relished the ability to spend so much quality time with my family.
The groundhog days of quarantine life were uneventful until one day when I felt the distinguishable pain of a collapsed lung. A few hours and an X-ray later confirmed my suspicion, and my doctor instructed me to go to the hospital. I was heartbroken as I looked into the eyes of my children, once again forced to leave them. If had known then just what truly lay ahead of me, I'm not sure I would have been able to go. That was the beginning of my never-ending pneumothorax and the harbinger to a completely unrecognizable life. It was the start of 123 consecutive days in the hospital. My pneumothorax wouldn't heal and my doctors were hesitant to intervene too much due to the problems it could create for transplant, and so I had no choice but to wait in the hospital, trying to balance my fragile and deteriorating health without letting my culmination of ailments send me plummeting to the intensive care unit.
Grateful my husband was allowed to stay with me but separated from my children, we would have brief, hour-long visits with them. Due to hospital COVID-19 regulations, our visits were segregated to the outside courtyard and our time was up almost as soon as it began.
My heart shattered a little more each time our visits were over, and visions of my children walking away will haunt me forever.
I hung pictures and twinkle lights in my room to make it feel like home. Embroidery and Game of Thrones distracted me. Nurses became like family. I wrote and read and always highlighted my days with what I was grateful for -- even something as small as good pancakes from the hospital cafeteria. I aimed to stay optimistic, believing that a positive mental state is just as important as the physical demands of staying strong entering into transplant. I let the phrase, “what's meant to be, will be,” guide me.
I was very isolated within my four tiny walls, with all hospital staff adhering to strict guidelines and limiting as much contact with me as possible in the hopes of protecting me from COVID-19. When it was decided that my floor was to become the new COVID-19 section, the smell of fear blew across the unit.
For 108 days, I wished for the perfect set of lungs, and the next day I got my call that there was a match.
After traveling a very far distance to reach me and eight hours in the operating room, my lungs were successfully transplanted two days later, after a year on the waitlist.
Finding the words to describe how I felt leaves me overwhelmed with how much I want to say, yet words feel too small in comparison to what I feel. I only hoped to one day be breathing easily and laughing with my family, reminiscing about those dark days saying, remember when, remember when, remember when? When your zest for life outweighs your fear of death, the reward is nothing short of magical.
Three months post-transplant and I am still amazed that it happened. My recovery in the hospital was excruciating but it went as well as we could have hoped for. Thinking of my fellow CF friends who took the same steps before me -- some more than once -- carried me through those arduous times, keeping me determined to get home to my children. And exactly two weeks later, I finally walked out of the hospital smiling and breathing deeply for the first time in many years.
This past year has been a barrage of unthinkables bookended by the greatest gift one could ever receive. The bittersweet taste of such a tumultuous year lingers for what I imagine will be forever. My days no longer consist of hours of breathing treatments and struggle, and instead laughter and ease. To think that there was a time when laughing would initiate coughing so severe that I would stop breathing is something I am so thankful to no longer identify with. And as the old saying goes, I can firmly agree that laughter is indeed the best medicine.
I think of my donor and his family every day. I carry him in all that I do. Because of him and his selflessness, my kids got their mom back. My husband got his wife back. My family got their daughter, sister, aunt, cousin, and niece back. Because of him, I got my life back.
I'm excited and hopeful for the future. Life post-transplant is more than I could have ever dreamed of. I have my children, my husband, my family, and the incredible air in my lungs. I'm not always sure where I am going from here, but the one thing I do know, is that I am forever grateful.
Interested in sharing your story? The CF Community Blog wants to hear from you.