With chest physical therapy (CPT), the person gets in different positions to use gravity to drain mucus (postural drainage) from the five lobes of the lungs. Each position is designed so that a major part of the lung is facing downward. When combined with percussion, it may be known as postural drainage and percussion (PD&P). This is where a caregiver or partner can clap and or vibrate the person’s chest to further dislodge and move the mucus to the larger airways where it can be coughed or huffed out of the body.
CPT is easy to do. For a child with cystic fibrosis, CPT can be done by anyone, including parents, siblings, and friends. It can also be done by physical therapists, respiratory therapists, or nurses during care center visits or in the hospital.
How to Do It
With postural drainage, the person lies or sits in various positions so the part of the lung to be drained is as high as possible. That part of the lung is then drained using percussion, vibration, and gravity. Your care team may tailor these positions to your or your child’s needs.
When the person with CF is in one of the positions, the caregiver can clap on the person’s chest wall. This is usually done for three to five minutes and is sometimes followed by vibration over the same area for approximately 15 seconds (or during five exhalations). The person is then encouraged to cough or huff forcefully to get the mucus out of the lungs.
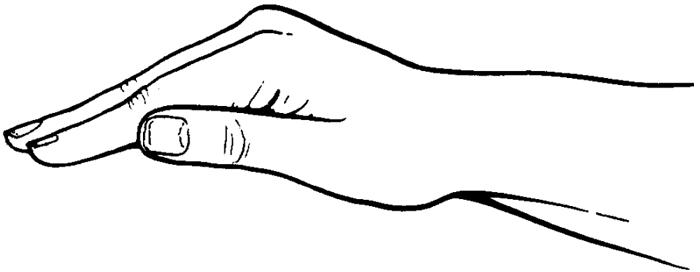
Clapping (percussion) by the caregiver on the chest wall over the part of the lung to be drained helps move the mucus into the larger airways. The hand is cupped as if to hold water but with the palm facing down (as shown in the figure below). The cupped hand curves to the chest wall and traps a cushion of air to soften the clapping.
Percussion is done forcefully and with a steady beat. Each beat should have a hollow sound. Most of the movement is in the wrist with the arm relaxed, making percussion less tiring to do. If the hand is cupped properly, percussion should not be painful or sting.
Special attention must be taken to not clap over the:
- Spine
- Breastbone
- Stomach
- Lower ribs or back (to prevent injury to the spleen on the left, the liver on the right and the kidneys in the lower back)
Different devices may be used in place of the traditional cupped palm method for percussion. Ask your CF doctor or respiratory therapist to recommend one that may work best for you.
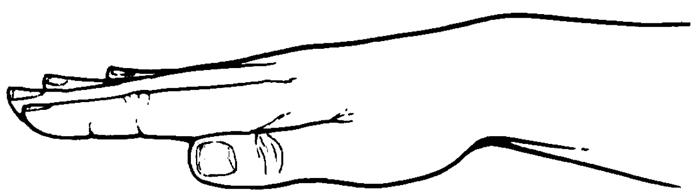
Vibration is a technique that gently shakes the mucus so it can move into the larger airways. The caregiver places a firm hand on the chest wall over the part of the lung being drained and tenses the muscles of the arm and shoulder to create a fine shaking motion. Then, the caregiver applies a light pressure over the area being vibrated. (The caregiver may also place one hand over the other, then press the top and bottom hand into each other to vibrate.)
Vibration is done with the flattened hand, not the cupped hand (see the figure below). Exhalation should be as slow and as complete as possible.
Deep breathing moves the loosened mucus and may lead to coughing. Breathing with the diaphragm (belly breathing or lower chest breathing) is used to help the person take deeper breaths and get the air into the lower lungs. The belly moves outward when the person breathes in and sinks in when he or she breathes out. Your CF respiratory or physical therapist can help you learn more about this type of breathing.
How Long Does CPT Take?
Generally, each treatment session can last between 20 to 40 minutes. CPT is best done before meals or one-and-a-half to two hours after eating, to decrease the chance of vomiting. Early morning and bedtimes are usually recommended. The length of CPT and the number of times a day it is done may need to be increased if the person is more congested or getting sick. Your CF doctor or respiratory therapist can recommend what positions, how often and how long CPT should be done.
Doing CPT Comfortably and Carefully
Both the person with CF and the caregiver should be comfortable during CPT. Before starting, the person should remove tight clothing, jewelry, buttons, and zippers around the neck, chest and waist. Light, soft clothing, such as a T-shirt, may be worn. Do not do CPT on bare skin. The caregiver should remove rings and other bulky jewelry, such as watches or bracelets. Keep a supply of tissues or a place to cough out the mucus nearby.
The caregiver should not lean forward when doing percussion, but should remain in an upright position to protect his or her back. The surface that the person with CF lies on should be at a comfortable height for the caregiver.
Many families find it helpful to use pillows, sofa cushions, or bundles of newspapers under pillows for support, as well as cribs with adjustable mattress heights/tilts, foam wedges, or bean bag chairs while doing CPT. Infants can be positioned with or without pillows in the caregiver’s lap.
Purchasing Equipment
Equipment such as drainage tables, electrical and nonelectrical palm percussors, and vibrators may be helpful. These can be purchased from medical equipment stores. Older children and adults may find percussors useful when doing their own CPT. Talk to your doctor or respiratory therapist at your CF care center about equipment for CPT.
Although insurance providers often do not cover equipment of this kind, check with your insurance provider for your specific plan’s benefits. Sometimes, companies that make this equipment offer assistance programs. Contact the company (or visit the company's website) for details.
You also can contact CF Foundation Compass, a personalized service that can help you with insurance, financial, legal and other issues.
Call Compass directly at:
844-COMPASS (844-266-7277)
Monday – Friday, 9 a.m. – 7 p.m. ET
compass@cff.org
Making CPT More Enjoyable
To make CPT more fun, consider one of the following:
- Schedule CPT around a favorite TV show.
- Play favorite songs or recorded stories.
- Spend time playing, talking, or singing before, during, and after CPT.
- For kids, encourage blowing or coughing games during CPT, such as blowing pinwheels or coughing the deepest cough.
- Ask willing and capable relatives, friends, brothers, and sisters to do CPT. This can provide a welcome break from the daily routine.
- Minimize interruptions. Finding ways that make CPT more enjoyable can help you keep a regular routine and get maximum health benefits.
"I firmly believe that I am better off for focusing on chest PT done manually by my dad ... It was a more personal connection. I wasn't sitting alone for an hour a day with a vest on. I know it's time consuming, but I think there's a value to it." — Chris Kvam, adult with CF
Instructions for CPT
The following diagrams describe the positions for CPT. In the diagrams, shaded areas show where the chest should be clapped or vibrated. As a reminder:
Pillows may be used for added comfort. If the person tires easily, the order of the positions can be varied, but all areas of the chest should be percussed or clapped.
Please remember to clap and vibrate only over the ribs.
Avoid clapping and vibrating over the spine, breastbone, stomach, and lower ribs or back to prevent trauma to the spleen on the left, the liver on the right, and the kidneys in the lower back. Do not clap or vibrate on bare skin.
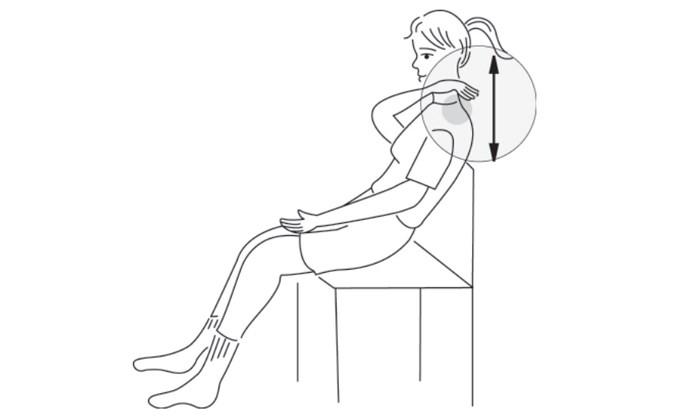
Self-Percussion — Upper Lobes
Your child should sit upright and reach across his or her chest to clap on front of chest over the muscular area between the collarbone and the top of the shoulder blade. Repeat on the opposite site. Your child can also clap his or her own upper back if able to reach it.
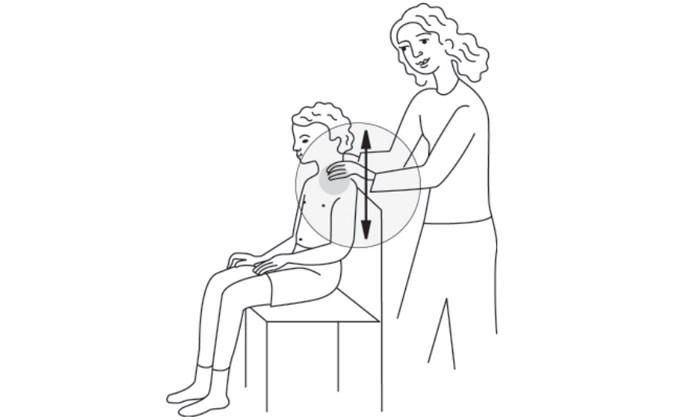
Upper Front Chest — Upper Lobes
Have your child sit upright. Clap on both sides of the upper front chest over the muscular area between the collarbone and the top of the shoulder blade.
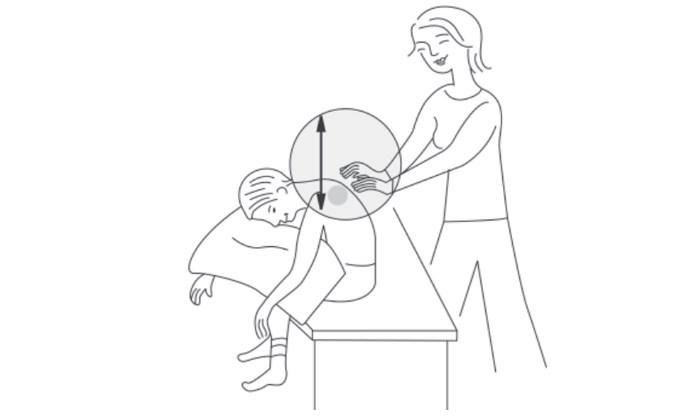
Upper Back Chest — Upper Lobes
Have your child sit up and lean forward on a pillow over the back of a sofa or soft chair at a 30-degree angle. Stand or sit behind your child and clap both sides of the upper back. Take care not to clap on your child's backbone.
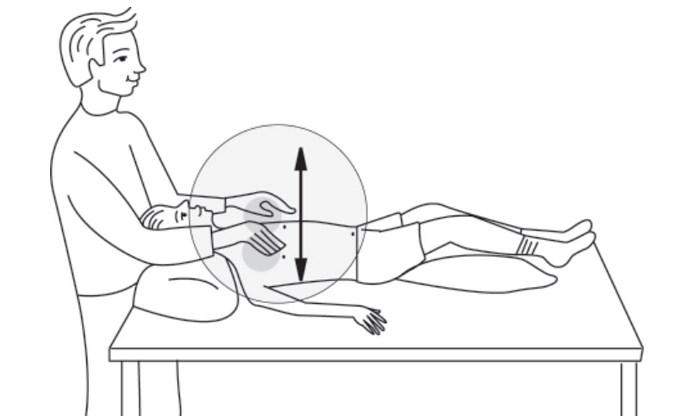
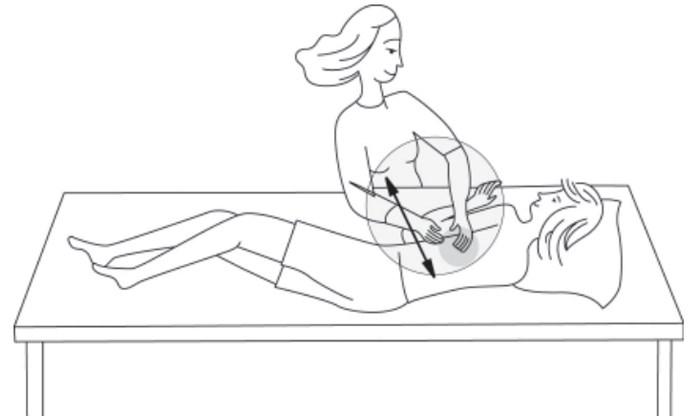
Upper Front Chest — Upper Lobes
Have your child lie on his or her back with arms to sides. Stand behind your child's head. Clap both sides of your child's chest between the collarbone and nipple.
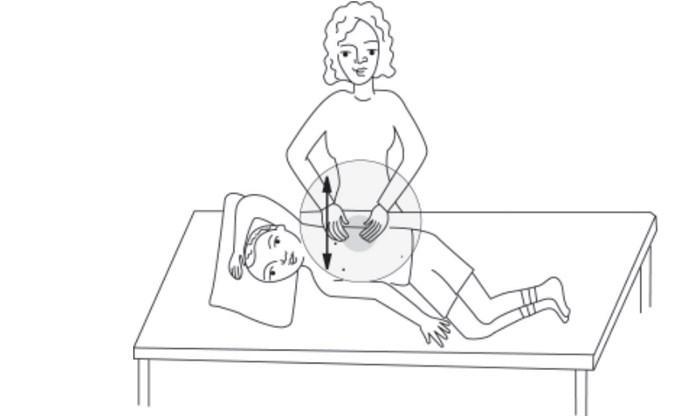
Left Side Front Chest
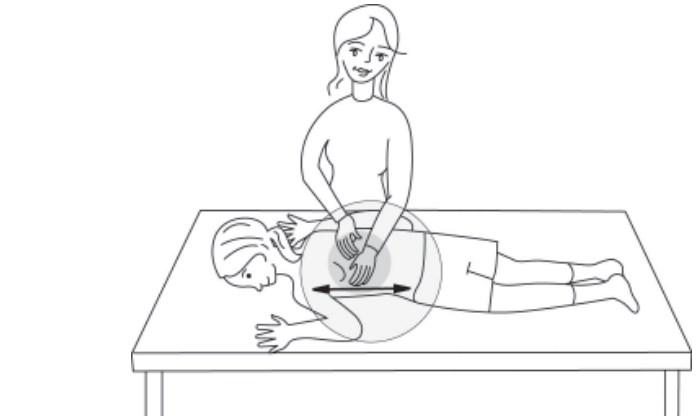
Have your child lie with left side up and raise his or her left arm overhead. Clap over the lower ribs just below the nipple area on the front side of left chest. Do not clap on your child's stomach.
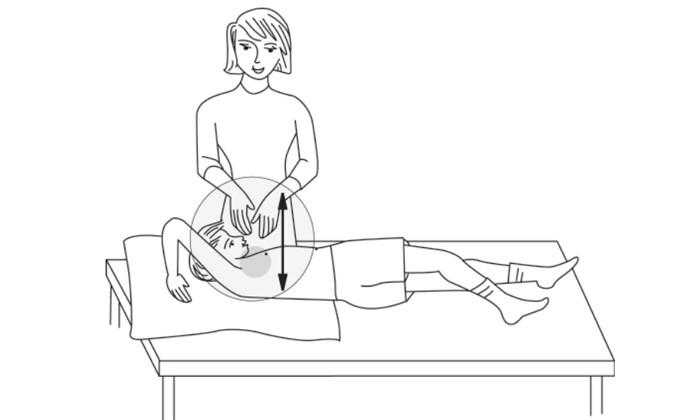
Right Side Front Chest
Have your child lie with right side up and raise his or her right arm overhead. Clap over the lower chest just below the nipple area on the front side of right chest. Do not clap your child's lower ribcage.
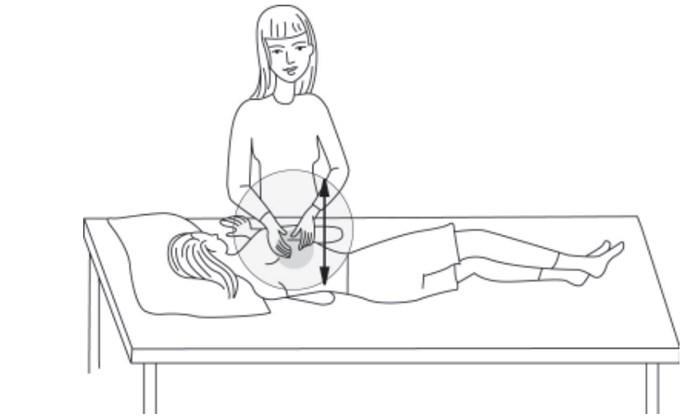
Lower Back Chest — Lower Lobes
Have your child lie on his or her stomach. Clap both sides at the bottom of his or her chest just above the bottom edge of the ribcage. Do not clap the lower ribcage or over the backbone.
Left Lower Side Back Chest — Lower Lobe
Have your child lie with left side up and roll toward you a quarter turn so you can reach your child's back. Clap on the lower left side of his or her chest just above the bottom edge of the ribcage.
Right Lower Side Back — Lower Lobe
Have your child lie with right side up and roll toward you a quarter turn so you can reach your child's back. Clap on the lower right side of his or her chest just above the bottom edge of the ribcage.
*Children shown without shirts to better demonstrate the PD&P technique in illustrations. Images are from the CF Family Education Program.