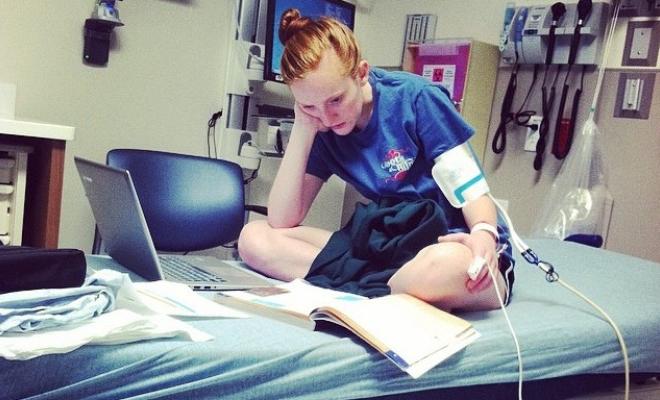
When Betsy was diagnosed at 18 months, my job was to be consistent with her treatments until the day she would take these tasks on herself. We all know, that as our young children watch us, we are teaching by our example. So we were compliant.
And as the years passed, new treatments were added because of a positive culture, new diagnosis or research supporting new therapies. When my daughter was 6 years old, she was diagnosed with CF-Related Diabetes (CFRD), which came with a new set of therapies and additional monitoring. But again, we forged ahead and in the back of my mind, I heard that still, small voice, reminding me that things will get easier once she is able to do these treatments on her own.
Betsy is 15 years old now. While she's managed all of her oral medications independently since childhood, I began to transition her to manage her other therapies when she was 11. She is fully capable of doing all of her treatments on her own. This includes tending to her port and daily IV therapy, managing her breathing treatments and airway clearance, monitoring her diabetes with insulin, setting up her feeding bag every night and taking the countless oral medications she needs daily. This is what I've been waiting for! She's a smart, funny, athletic kid with countless true friends. She's on the honor roll and excels in sports. What I did not count on, is her teen rebellion.
While at a Parent Teacher Organization meeting, I was biting the inside of my cheek and pinching my upper arm as I listened to other parents complain about their teens turning assignments in late, not cleaning their rooms, or not keeping track of their athletic uniforms. I wanted to scream. What I wouldn't do for Betsy to rebel like that! Instead, my child, who has always been so well versed in her treatments (I recall her calling out a nurse about improper dosing of heparin when she was 3 years old) was not just skipping treatments, she was actually resisting them.
Teenagers rebel. That's what they do. What I've learned is that anger and rebellion go hand in hand.
And she's mad. I don't blame her. CF is miserable. This makes perfect sense. The harder I push, the more she resists.
I read the blogs and stories parents write about their compliant CF kids, I hear CF adults speak about never missing a treatment or medication, and despite my best efforts, I am fighting a battle I never imagined with Betsy. If I've learned nothing else, it's to wave the white flag before I need it. For me, that meant getting the support of Betsy's team of clinicians.
I am fortunate that Betsy is part of a comprehensive care team. The same doctor who talked to me 14 years ago was ready, willing and able to step in. Her team was eager to support her. They've seen this before and have the experience and tools to work with her. By meeting her anger with compassion, her resistance with compromise and her excuses with gentle explanations, we are turning a corner.
They've taken much of the weight off of my shoulders. They send Betsy emails encouraging her. They've also reassured me that this is not uncommon and that it's not my fault.
I'll never forget what my 3-year-old said after Betsy was diagnosed. Her world was turned upside down. She was forced to sit and watch as Betsy did her treatments and I beat on her little body as part of her therapy. She said, “Mama, I'll take some of Betsy's roses, but I don't want all 65 of them." I totally get that.
Fitting the demands of CF therapies into any schedule is challenging. As children and adolescents, most patients are able to somehow juggle this with their parents' support. But when that responsibility shifts to patients who are also faced with many other new challenges, it can become an overwhelming burden. High school, sports, friends and classes are the priority now for Betsy. Finding the support needed to help manage this complicated transition is critical to her health. The easy thing would be to do nothing and hope that she finds her way. Asking for help is hard. But being in the foxhole alone is even harder.