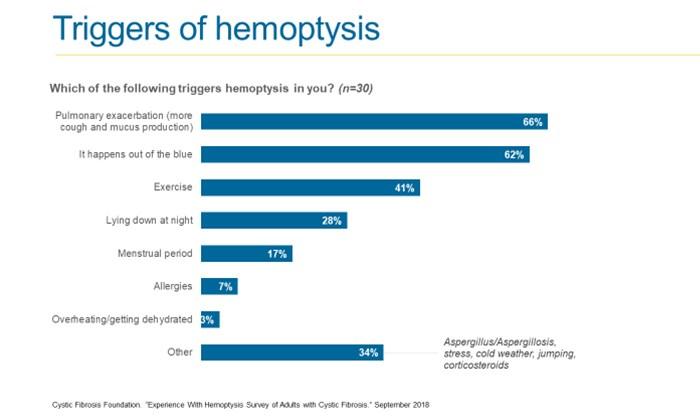
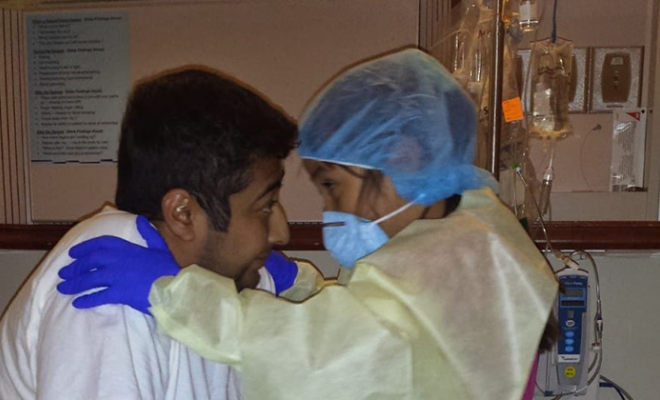
Last year, Dr. David Orenstein wrote a blog post that put hemoptysis in a medical perspective. In the grand scheme, it doesn't happen often and when it does, it isn't typically dangerous. But there are statistics, and then there is lived experience. When the Cystic Fibrosis Foundation surveyed people with CF in Community Voice (including me) about their experiences with hemoptysis, the responses varied widely. But when it's happening to you, knowing what hemoptysis could look like can help you handle it.
For those of us who have experienced it, hemoptysis is gross. It's scary. It might even be embarrassing. But, it can also be a fact of life when you've got cystic fibrosis like I do. The first time I coughed up blood, it was just tinges in my sputum. It happened when I was starting a new inhaled antibiotic and beginning to use the Vest®. I was just 20 years old and I was scared. My care team was great though, and when I told them what had happened, they told me to stop using the Vest until my body got used to the antibiotic and then restart. Evidently it was just too much change for my lungs all at once.
Fast forward a few years and I'd just been admitted to the hospital for an exacerbation brought on by a nasty virus my husband and daughter had generously shared with me. I coughed up pinkish mucus, which then became mucus with red streaks. I showed my respiratory therapist (RT) who reported it to the rest of my care team.
During all of that, my doc came and sat down with my husband and me and had to have a serious talk. He wanted to prepare me for the possibility that coughing up blood was something that could happen again. It was scary to hear that coughing up blood could be as minor as what I'd just experienced, or as major as spattering blood all over myself and my room and having to be taken by ambulance to the nearest hospital for an embolization. However, the next several times I experienced hemoptysis, he repeated the same information:
- If you're home, stop your treatments until you call us. We can help you figure out a game plan.
- Spit into a cup, so you can estimate the amount of blood you're bringing up and how quickly.
- If you're bringing up too much blood too quickly to measure, call an ambulance and try to lie with the lung you suspect is bleeding facing the floor.
Even though I hated these talks and they really scared me, I'm so thankful for them. When I did cough up a lot of blood at home, splattering the book I was reading, my hands, face, and shirt, I knew what to do.
I grabbed a cup, kept an eye on the clock to measure how quickly I was filling the cup, called my care team, and alerted my husband in case it got worse. I was scared, but I was also prepared.
Hemoptysis can vary so widely from person to person that it's hard to say exactly how it's going to feel or look. You might have pain and know where your bleeding is coming from, or you may not even know you're coughing up blood until you see it in a tissue or cup. But, that variance is exactly why it's a good idea to have conversations with your care team to know what you should expect and how to be prepared. It might seem like a better idea to just put it out of your mind and not worry if it hasn't happened to you, but sitting on your fear or playing ostrich isn't going to prevent hemoptysis from happening to you.
Whether it is something you have dealt with, or will deal with in the future, being prepared gives you the power to take control of a situation that can make you feel totally out of control. If that moment ever comes, you can grab hold of your plan instead of scrambling around in fear.
Your doctor may not bring it up like mine did, but that's okay. You should feel empowered to bring up anything that concerns your health. You can ask questions based on things you've read or heard. You're the one who has to manage this disease all day every day and that means you need to know about contingencies like coughing up blood, even if it's not something that's ever happened to you. You might consider asking your team:
- Should I be concerned about hemoptysis?
- What should I do if it happens to me?
- Are there things I can do to prevent it?
- What about this research that I've read? (Bring the article, if possible.)
There are lots of things about CF that aren't pretty or glamorous and coughing up blood is one of them. However, there's no reason to be ashamed of it and you have every reason to be informed. There are a lot of things we still don't know about hemoptysis. Are there certain drugs, bacteria, environments, activities, or other factors that make it more likely to happen? Does a woman's menstrual cycle make it more likely to happen? Are women with CF more at risk than men?
We don't know the answers to these questions yet, but hopefully more research will bring us answers. In the meantime, work with your care team to make sure you're the best-prepared CF patient that you can be! You deserve it.