Most hospital admissions are unpleasant; you are put in a room where the bed isn't comfortable, the sheets are scratchy, and you're hooked up to monitors and machines that continually check your vitals.
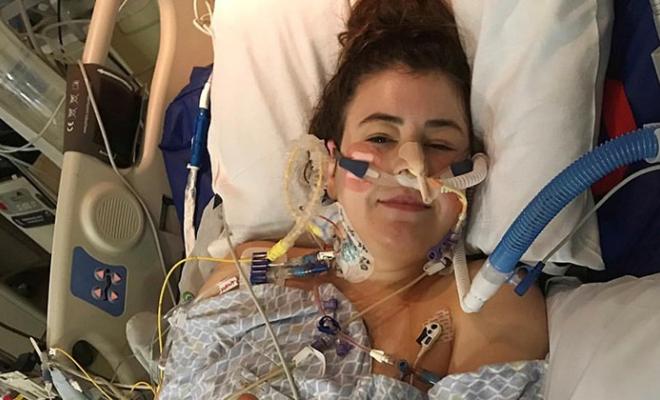
But back in February 2018, none of these typical hospital visit frustrations even registered with me. A simple cold had wreaked total havoc on my body and my already damaged lungs. I was in so much pain, I wasn't even annoyed that I had to go to the emergency department.
Through choking sobs, I laid on the gurney and began explaining to my mom that I started coughing uncontrollably, couldn't catch my breath, and started to have a panic attack in the middle of the night. It was such a traumatic experience, as I'd never suffered panic attacks before. My worst fears overwhelmed my brain and I didn't know how to stop myself from spiraling completely. It took me a while to finally calm down as I continually told myself that I was going to be okay … it was all going to be okay … but my nerves were shot, and I was completely depleted physically and mentally.
https://www.instagram.com/p/BfeYKlAlOQK/?taken-by=saltywoman65
I was in the hospital for a total of 15 days -- almost 10 of which I had high fevers that left me without an appetite. I ended up losing close to 10 pounds and became very weak. I could only take short walks and they left me exhausted and short of breath -- even showering became tiring.
This unexpected turn in my disease left me feeling anxious about what my life would now look like.
I began by sharing my worries and feelings with the CF psychologist on my care team. After our talk, we decided it would be wise for me to start taking a medication to help with anxiety. Although I was nervous about taking an anti-anxiety medication because I didn't want to feel like a zombie or be totally checked out, I was reassured this wouldn't happen, and have been able to manage my anxiety much better. Occasionally, I still get “mini” panic attacks, but when this happens, I go through breathing exercises and just have to repeat to myself that I am going to be okay.
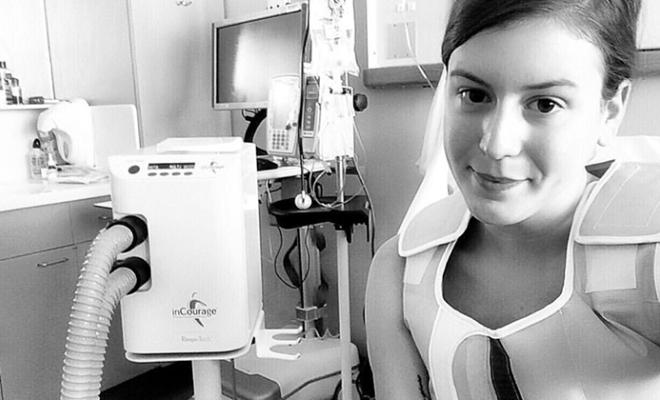
I've also been on supplemental oxygen for several months and will be indefinitely. It has been a challenge adapting to my “new normal.” For starters, I never realized how much freedom I had until I was placed on supplemental oxygen.
Before, if I needed to go to the grocery store, I could just grab my purse, keys, and reusable bags and head out the door. Now, I have to make sure my portable oxygen concentrator battery is charged enough to last me the whole time I'm gone. I also become fatigued a lot faster, which is why now I must try to space out appointments, activities, and time with family and friends because I need a day in between to recover and rest.
In addition, I have to fill out special paperwork and get permission from my doctor stating that it is safe for me to travel by air, and make sure that I have enough batteries for my portable oxygen concentrator to last the entire flight since liquid oxygen tanks are not allowed onboard.
I'm still trying to figure out my new normal, and I'm constantly fixing my nasal cannula and getting tangled up in oxygen tubing. But, like everything, I know that it won't be this way forever. For now, I am just going with the flow and riding the wave we call life.
Join the conversation on Facebook.