People with cystic fibrosis face unique challenges before and after any surgery, but the internet has a dearth of information about these challenges, especially as they relate to liver resection surgery (surgery to remove part of the liver), so I want to share my experiences and lessons learned with others with CF who may be facing surgery. Having realistic expectations and being a good self-advocate make the recovery process a little easier.
- CF may not be your only health challenge. I was facing liver resection because a magnetic resonance imaging (MRI) scan revealed that I had what appeared to be an adenoma, a type of tumor, in my liver. Being diagnosed with a liver problem unrelated to CF made me realize that CF didn't protect me from having other unrelated health challenges. This seems obvious, but it's easy to get tunnel vision and only focus on CF. It turned out that the lump in my liver was not an adenoma. Rather it was a “focal fatty change” -- a large lump of fat -- caused by having CF. Although my liver problems did turn out to be CF-related, I still think this is an important lesson to learn.
- Get plenty of rest. After I learned that I would need surgery, I spent the next two weeks going to doctors' appointments, undergoing tests, planning for my absence from work, and learning as much as I could about the surgery. During this time, I worried that the stress of my situation might make me sick and force me to reschedule the surgery. To prevent this, I tried to get as much sleep as possible.
- Ask questions and be prepared for surprises. On the day of the surgery, the anesthesiologist explained my pain management options and told me that although they would do everything possible to help me, I would be in a lot of pain after the surgery. He also told me that the pain medication could cause nausea. I was surprised, because pain and nausea had never been mentioned to me before. I expected fatigue but not a lot of pain. Learning this new information with less than an hour before surgery didn't allow me to mentally prepare for how difficult recovery would be.
I was angry during the first days of recovery because of how different my experience was from what I had expected, and I spent a lot of precious energy processing all the unexpected experiences. Having realistic expectations would have let me focus my energy on recovering, and I would have been a lot nicer to be around.
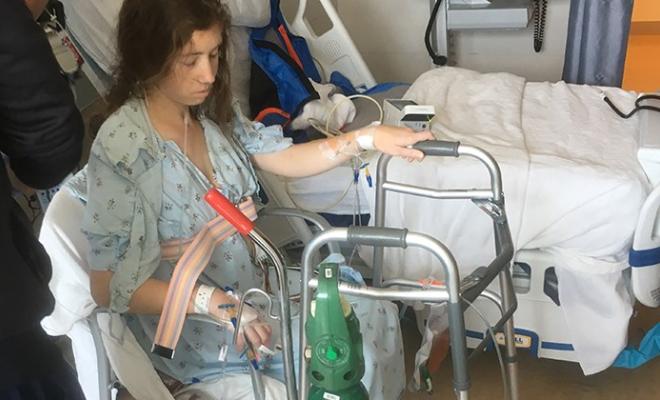
I also found out that my gallbladder would be removed. To avoid this kind of surprise on the morning of the surgery, I recommend patients ask their surgeons to walk them through everything they will be doing during the surgery prior to the day of the surgery. - Don't compare yourself to others. The anesthesiologist was right, I had pain after surgery. My first walk post-surgery was the most difficult thing I've done in my life. The nausea, fatigue, and pain made it seem like a herculean task. When I told my physical therapist that I felt badly about struggling and complaining when the other patients on the floor, many of whom were recovering from liver transplants, must be feeling much worse, he told me that their pain didn't take away from mine; what I was feeling was real and challenging. I believe this is important to remember as we hear stories or see others struggling with health issues. Feeling guilty about having smaller challenges than another person isn't helpful for either person.
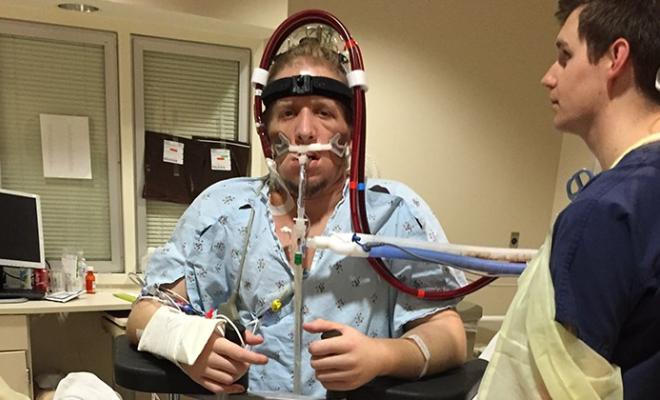
- Commit to airway clearance. After the surgery, breathing was challenging. The pain of breathing caused me to take shallow breaths. At times I felt like I was getting worse, and even brought up bloody mucus after a couple of days. I learned that no matter how tired I felt, I needed to keep using the incentive spirometer and an Aerobika® every hour to keep my lungs as open as possible and my temperature from turning into a fever. Being disciplined about this started to make me feel better. Over the next few weeks I slowly regained my lung function and could take deeper breaths.
- Be your own best advocate. While I was in the hospital, I was followed by both the liver and pulmonary teams. There were no CF doctors at the hospital, so the pulmonologists conferred with a CF doctor at a different site. It was scary to be having problems with my lungs and not have a CF doctor nearby. I was also concerned that they didn't seem concerned about me coughing up blood and having a hard time breathing. I didn't learn until later that they were actually quite concerned that I would get pneumonia. Knowing that they did care and were concerned about me made me feel safer. I could have saved myself this stress by asking more questions, voicing my concerns, and asking what their plan was and what treatment options were available. Also, having a notepad and designated writer helps prevent questions from being forgotten when the doctors make their rounds.
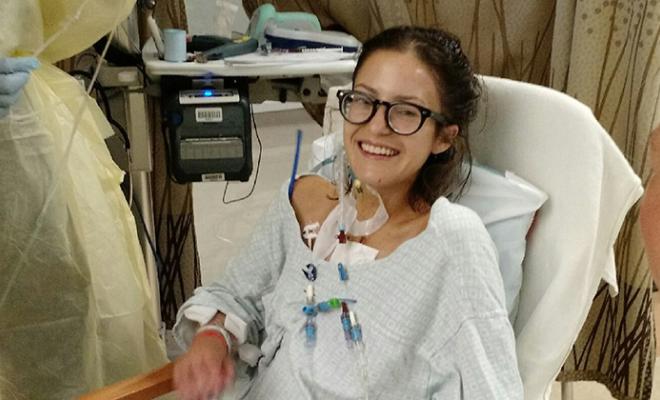
- Have social support in place. Having physical and emotional support from my family and friends made a huge difference in my recovery. From bringing me food to helping me in and out of bed to walking with me and keeping me company, they made me feel cared about and more connected to the outside world. The recovery process is long -- I wasn't able to return to work for six weeks, and I was still not 100 percent -- so having supportive friends and maintaining social interactions is important for mental health.
- Reflect on your progress. Recovery had its ups and downs. Reflecting on each day and finding one marker of progress helped, even if some things happened during the day that made me feel like I was going backwards or not making progress. The progress could be something as simple as setting a new personal best for how high I could get the gauge on the incentive spirometer or being able to sit in a chair for a longer time. Recognizing my progress every day helped me feel more optimistic about my recovery.