In recent years, mental health has become a more common component in the overall care of patients with cystic fibrosis. Reading stories from adults with CF, I learned most could recall the exact incident and age of their first negative experience, which shaped their mental health before they reached age 5.
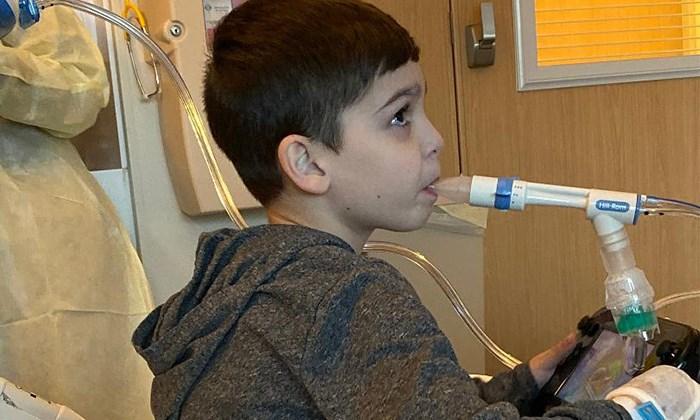
My son had a very difficult start in life that required antibiotics every month, four treatments a day for months on end, many hospitalizations for pulmonary exacerbations, as well as tests and procedures to determine severity of reflux, significant stomach pain, and digestive issues that weren't responding to typical treatment and routine care. All of this shaped his perception of cystic fibrosis and hospitals and, in turn, negatively impacted his mental health.
By the time my son was 3 years old, I saw a dramatic, adverse change in his behavior. He was able to verbalize his thoughts and feelings and what led to this change, and I learned it all stemmed from medical trauma.
I immediately reached out to professionals inside and outside of our CF clinic to understand more of what was going on and how I could help my son. I was saddened to learn that mental health was not well addressed or screened for children with CF until they reached 12 years old.
While getting my master's degree in education, I studied the cognitive, social, and emotional development of children in depth. Significant trauma can greatly impact a child's mental health well before the age of 5, and I saw that firsthand with my own child. I constantly championed medical professionals who were treating my son and gave examples of how medical procedures harmfully impacted a child's mental health from an early age. Depending on the severity of the disease, a child with CF could experience more before the age of 5 than some kids with CF experience before they reach their teenage years.
I encountered medical professionals with varying degrees of bedside manners and advocated many times for what I thought was best for him. I wish I could say it was an easy battle, but it wasn't by any means.
Too often, I kept hearing he won't remember these moments, and he'll become less anxious and more compliant as he grows older and has a better understanding of the tests and procedures.
Addressing the mental health of a toddler is not easy since they have limited cognitive understanding of their own emotions. I searched for and interviewed countless therapists until I found someone I thought was right for my son. I decided on a therapist who worked with cognitive behavioral therapy because I like that it is based on developing coping strategies. Being an educator, I see the importance of children learning and using coping strategies from an early age.
With the help of therapy, I was able to teach my son how to self-advocate starting at age 4. I learned what prep time meant for him when it came to specific procedures and appointments coming up. He knows procedures are non-negotiable, but he has learned how to stand up for himself and effectively communicate what he needs from his CF team and other medical professionals.
He has learned how to recognize his anxiety triggers. I learned his “tells” so I could continue being his best supporter and advocate. We have come up with scenarios and game plans on how to handle anxious moments in medical circumstances. It's a constant work in process and always changing based on his age and stage, but I am proud of my son in how far he has come and what he has learned.
My son is 8 years old now. I know I can't remove cystic fibrosis from his life, but I can give him the tools he needs to cope with the challenges that come from living with this disease.
Interested in sharing your story? The CF Community Blog wants to hear from you.