Having cystic fibrosis and other chronic illnesses means that I’m often not feeling my best. I spend many days lying around the house bemoaning my plight — complaining about how tired and miserable I am. I miss out on important moments in the lives of my family and friends. Too often I must reschedule or cancel my appointments with my clients and step back from the nonprofit practice that I helped create.
My core values include love, loyalty, family, friends, responsibility, independence, integrity, and adventure. It’s very hard for me to stick to my core values when I have no energy to take care of myself — much less take care of others. Being a good mom, wife, friend, and therapist means I must be able to be present and supportive — which is almost impossible when I’m exhausted. A huge part of my identity is tied to being a trustworthy caretaker.
My sense of self-worth is tied to how well I help others and how much they can depend on me. Consequently, I feel worthless and powerless when I’m unable to tend to those I cherish. It leads to feelings of melancholy and frustration. Not living up to my expectations and values is rough. It sends me down the dark, dangerous path toward depression and anxiety.
It’s tough to feel happy with a hurting body and the chance that it might not get better. It’s challenging to feel content when we’re so often isolated from others or stuck in a sterile hospital away from our loved ones.
Feeling like a burden to others is also a very unpleasant experience. Especially if you’re like me and want nothing more than to be healthy and present in the lives of those we love. Many of us want to work and contribute to the world around us, but it’s very hard to do that when we can’t breathe or are physically and mentally exhausted — or, if you spend copious amounts of time in the bathroom every day like I do. Gross, but so true for many of us with CF.
It can be so hard for me to participate in events outside of my home or even do telehealth with my clients because of my digestive problems. Among all the medications I take, dietary restrictions, breathing treatments, and GI issues, it’s hard to do much else other than take care of myself. I currently need people to help me care for myself — and that’s very hard for me. I don’t like the shoe being on the other foot so to speak. I prefer to be the caretaker, not the patient.
Those of us with CF or other chronic illnesses understand what I mean when I refer to “good days” and “bad days.” A “good day” is a day with less pain, higher motivation, and more energy. A “bad day” is a day when it’s hard to get out of bed, get dressed, brush your teeth, and participate in daily activities due to illness.
Lately, I’ve had fewer “good days” and more “bad days.” I’ve recently felt as though I’m a half-human who doesn’t get to participate in the world inhabited by other, normal human beings. It’s hard for me to articulate exactly what I mean but it’s like existing without purpose. Like there’s this invisible barrier — a fog — that separates my bedroom from the rest of the world. A haze that makes it difficult to see beyond my exhaustion, sickness, and loneliness — a miasma that my physical and mental pain has manifested that bars me from being a fully-functioning human being. But once that fogs lifts, I’m able to see beyond my pain.
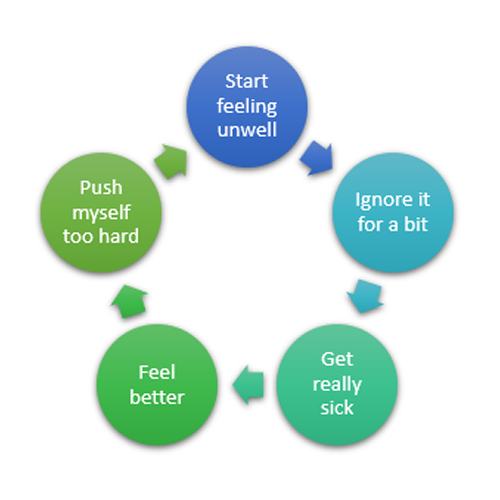
It's exciting and invigorating to feel better — to feel as though I can live fully again — so I try to catch up on all the things I missed out on when I wasn’t feeling my best. Since my good days have been decreasing in frequency, when I have a good day, I want to take advantage of it. I want to show my son with CF-related metabolic syndrome that life with a CFTR disease can be wonderful and have fun with him. If I missed some of my loved ones’ birthdays, no problem, I’ll make it up to them today. No holds barred. I want to experience LIFE on my good days.
The problem is that I often go too hard on my good days and end up creating more bad days for myself. Then, I feel even more frustrated and disappointed in myself. My attention-deficit/hyperactivity disorder (ADHD) brain doesn’t help either because often it tells me to do things without thinking. So, I end up back at the doctor’s office, hospital, or lying on the couch in that half-alive state I so despise.
So, how do I stop this cycle? I start by listening to my body. I listen to my doctors, therapist, and nurses, when they tell me to rest, to take things slow when I start to feel better. Life isn’t a half-life when I’m in bed sick. It’s simply my life living with CF. It’s my reality. I try to practice radical acceptance, which is the practice of accepting life as it is and coping with challenges in healthy ways and accepting that life has meaning despite its challenges. Finding meaning when I feel meaningless is difficult. It’s not impossible, though.
Those days when I’m stuck on the couch or in bed sick are when I talk to others experiencing chronic illness online and I check in with my friends, family, and clients on my phone. I accept that I need help myself sometimes and that it doesn’t make me a burden. Video conferencing technology enables me to live in the moment with others, even if I’m not feeling physically present. I don’t ignore the uncomfortable feelings in my body and mind, but I also try not to get lost in them. After all, depression and anxiety are always waiting for me. I try to utilize healthy coping mechanisms to address my hurt — although I’m not always successful. I acknowledge my pain and I sit with it for a bit.
Interested in sharing your story? The CF Community Blog wants to hear from you.