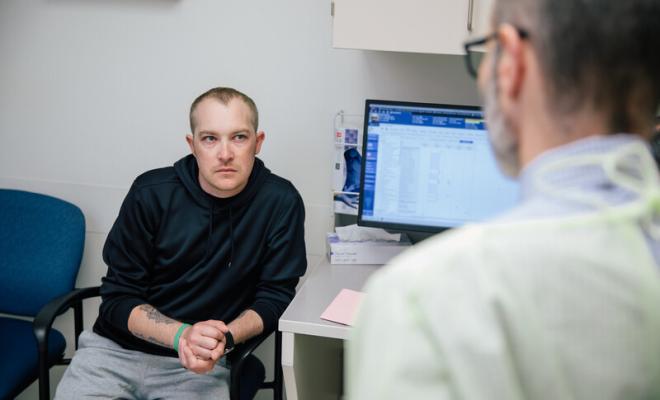
Models of Palliative Care Delivery for Individuals with Cystic Fibrosis
Kavalieratos D, Georgiopoulos AM, Dhingra L, et al. Models of Palliative Care Delivery for Individuals with Cystic Fibrosis: Cystic Fibrosis Foundation Evidence-Informed Consensus Guidelines. J Palliat Med. 2020 Sep 16. doi: 10.1089/jpm.2020.0311. Epub ahead of print. PMID: 32936045.
Purpose/Background
Palliative care has been shown to be effective in alleviating distress and discomfort and enhancing quality of life in a variety of patient populations (e.g., cancer, heart failure, HIV); however, its integration into cystic fibrosis care delivery has neither been effectively studied nor implemented. The Cystic Fibrosis Foundation convened a 22-member committee, composed of CF clinicians, palliative care specialists, adults with CF, caregivers, researchers, and administrators, to develop recommendations based on the literature and expert opinion consensus. The committee established the following definition of palliative care that drove their subsequent work: ‘‘Palliative care focuses on reducing physical and emotional symptoms and improving quality of life for people with CF throughout their lives. Palliative care occurs alongside usual treatments and is individualized according to the unique goals, hopes, and values of each person with CF.’’
- Primary palliative care: These services include, but are not limited to:
- Managing patients’ pain and other physical and emotional symptoms.
- Engaging in discussions about goals of care with patients and caregivers.
- Exploring options for life-prolonging treatments in cases of respiratory failure.
- Identifying a health care proxy.
- Guiding development and documentation of advance directives.
- Educating and supporting patients and caregivers on discussions of transplantation, including medical indications, processes, and outcomes.
- Specialty palliative care: These services include, but are not limited to:
- Assisting with management of physical and emotional symptoms refractory to primary palliative care interventions.
- Addressing existential/spiritual distress of patients or caregivers.
- Discussing code status, advance directives when there are misunderstandings of options, and prognosis.
- Facilitating resolution of discordance among patients, caregivers, and health care providers, including misalignment of goals of care and treatment decisions.
- Exploring wishes around end-of-life care.
Methodology and Results
Between July 2018 and August 2019, the committee:
- Collaborated with a health sciences librarian to extract extant literature.
- Reviewed and assessed each reference for relevance.
- Developed and revised recommendation statements.
- Voted on the recommendation statements with an 80% threshold for acceptance among member recommendation statements.
- Developed a draft of recommendation statements that were subsequently released for a two-week public comment period via an internet-based survey.
The initial literature search yielded 8,465 references, of which 340 full-text articles were reviewed. A final yield of 116 articles were appraised as relevant. From the comprehensive literature review, 11 recommendation statements were developed, which were organized into three categories:
- Primary palliative care, with 5 recommendation statements.
- Specialty palliative care, with 3 recommendation statements.
- Screening and assessment of palliative care needs, with 3 recommendation statements.
Out of the 11 recommendation statements, the following are the primary recommendations that are most critical and relevant to CF clinicians.
Primary Recommendations
For all recommendations and further detail, please see the published manuscript.
|
Recommendations |
Evaluation of the Evidence |
| The CF Foundation recommends that CF care teams deliver primary palliative care as part of usual CF care, at the time of diagnosis and throughout the disease course. | 100% Consensus |
| The CF Foundation recommends that CF care teams partner with specialists who are consulted to assist with palliative care needs to facilitate the specialists’ understanding of CF care and the unique needs of individuals with CF. | 100% Consensus |
| For individuals with CF ages 12 years to adulthood, the CF Foundation recommends using the IPOS, annually and at disease milestones (e.g., changes in disease severity, functional decline), for screening and clinical assessment of unmet palliative care needs. | 100% Consensus |
| For children with CF under age 12 years, the CF Foundation recommends using the IPOS to guide conversations with children and caregivers, annually and at disease milestones (e.g., changes in disease severity, functional decline), to identify unmet palliative care needs. |
100% Consensus |
| For caregivers of individuals with CF of all ages, the CF Foundation recommends offering screening to at least one primary caregiver annually and when disease milestones (e.g., changes in disease severity, functional decline) trigger repeated screening, using the BASC. | 100% Consensus |
Unanswered Questions
- How does CFTR modulator therapy affect patients’ and caregivers’ palliative care needs?
- What is the ideal model for palliative care in the pre/peri/post lung transplantation trajectory?
- What is the role of palliative care to support individuals who are either ineligible for, or decline high-impact, life-saving therapies like lung transplantation or modulator therapy?
Updates
- Trandel ET, Pilewski JM, Dellon EP, et al. Prevalence of Unmet Palliative Care Needs in Adults with Cystic Fibrosis. J Cyst Fibr. 2020. 19(3): 394-401. doi:https://doi.org/10.1016/j.jcf.2019.11.010.
- Lange AV, Rueschhoff A, Terauchi S, et al. End-of-Life Care in Cystic Fibrosis: Comparing Provider Practices Based on Lung Transplant Candidacy. J Pal Med. doi: http://doi.org/10.1089/jpm.2019.0304
Resources
- Improving Life with CF hosts palliative care screening and care provision workflows, best practices guides, and educational materials for clinicians and people with CF and their families.
Use of These Consensus Recommendations
The CF Foundation intends for this executive summary of its consensus recommendations to summarize the published consensus recommendations. The published consensus recommendations summarizes evidence, and provides reasonable clinical guidance based on that evidence, to clinicians, patients, and other stakeholders. Care decisions regarding individual patients should be made using a combination of these recommendations, the associated benefit-risk assessment of treatment options from the clinical team, the patient's individual and unique circumstances, as well as the goals and preferences of the patients and families that the team serves, as a part of shared decision-making between the patient and clinician.
This executive summary was prepared by:
Sigrid Ladores, PhD, RN, PNP, CNE, FAAN (Department of Family, Community, and Health Systems, School of Nursing, University of Alabama at Birmingham, Birmingham, Alabama) and Dio Kavalieratos, PhD (Division of Palliative Medicine, Department of Family and Preventive Medicine, Emory University, Atlanta, Georgia)