Although consistently taking medications (or adherence) is crucial for better health, it doesn’t tell the whole story. For many people with cystic fibrosis, it is difficult to balance a busy life with daily CF treatments. People with CF face a heavy treatment burden, and there are many barriers that can get in the way of sticking with their care. On average, people with CF only take half of their prescribed medications, and that percentage can be lower for individual therapies.
Reframing Adherence: What Is Partnerships for Sustaining Daily Care?
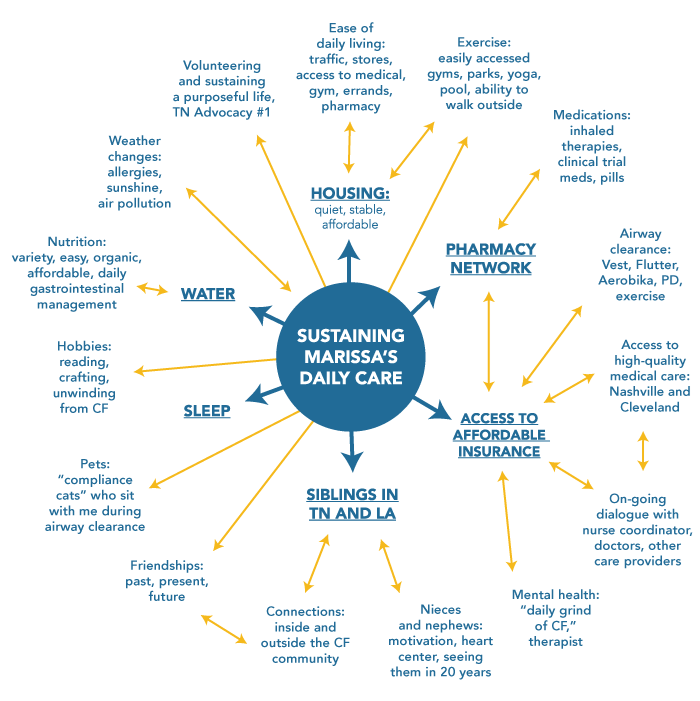
Cystic fibrosis can affect many aspects of people living with the disease. Each aspect can represent a barrier to sustaining daily care, including financial and emotional issues. A person's life stage, personal values, and goals can all also affect their ability to manage their daily care.
Recognizing these challenges, the Cystic Fibrosis Foundation made a strategic commitment to develop a multi-pronged approach to help people with CF stick with their treatment plans called Partnerships for Sustaining Daily Care (PSDC). The goal of PSDC is to bring together individuals with CF, their families, and care teams to foster productive conversations about aligning personal goals with health goals.
To inform this strategic initiative, a group of representative experts in CF care formed an advisory committee. This special committee worked together to understand the perspectives of all those involved in CF care. Each brought a unique perspective and experience that complemented and helped shape the discussions.
| Advisory Committee | Perspectives Contributed |
|---|---|
| Adults with CF | Insights into the daily realities and treatment burden of the disease while navigating the health care system |
| Parents of children with CF | Insights into the burden and systemic challenges from the perspective of parent caregivers |
| Nurses | An understanding of the coordination of care, education, and self-management skills on behalf of the multidisciplinary care team |
| Nurse practitioners | An understanding of the coordination and direct provision of care, education, and self-management skills on behalf of the multidisciplinary team |
| Physicians | Insights from clinicians who are the primary directors of medical recommendations and leaders of multidisciplinary care teams |
| Pharmacists | Pharmacological expertise of medication efficacy and knowledge of drug-to-drug interactions that impact a person's ability to manage their care |
| Respiratory therapists | Knowledge of the respiratory implications of CF, along with the dynamics of the multidisciplinary care team |
| Registered dietitians | Understanding of the nutritional aspects of CF and the dynamics of the multidisciplinary care team |
| Social workers | Knowledge of the psychosocial needs of individuals living with CF, as well as how to navigate insurance and access processes to ensure the ability to sustain daily care |
| Psychology researchers | Ability to formulate research questions to conduct rigorous studies and uncover insights into behavior |
| Pharmacy representatives | Insights on the challenges of physically and financially accessing medications and supportive medical devices |
| Pharmaceutical companies | An understanding of the challenges of development, marketing, and financial coverage of medications |
Their work has culminated in a critical shift: moving away from a discrete focus on increasing “adherence” to prescribed medications and moving toward a more comprehensive approach of supporting “partnerships for sustaining daily care.”
This shift to partnerships to sustain daily care relies on two core ideas.
Complementary Expertise
Care teams have medical and evidence-based knowledge of the disease and treatments, and can share experiences from treating other patients. People with CF and their families have expertise in how the disease affects them and how the context of their daily lives can affect how they approach their care. By acknowledging these respective roles, people with CF, their families, and care teams can work together to develop treatment plans that align personal life goals with health goals.
The first thing I remember after waking up from [lung transplant] surgery was my inability to talk. I knew that I would wake up connected to a ventilator and that the best way to communicate would be through writing. … I asked questions. … I even reminded my nurses about my insulin and other essential medications. I learned that I could still be my strongest advocate without even speaking. -- An adult with CF
Partnerships for Sustaining Daily Care: One CF Team
Shared Humanity
Each of us struggles to make decisions that involve tradeoffs within the context of our daily lives. Daily care does not happen in a vacuum. Recognizing that we all have challenges in doing “what is best for us” is more likely to foster honest, non-judgmental, problem-solving conversations about daily CF care plans.
… as long as what you say doesn't come off as sounding judgmental and sometimes even [showing that you understand how difficult their daily routine is by] saying to people 'Oh my gosh, all I have to do is take my vitamin every day and I can't even do that.' Sometimes it's empathizing with them and saying, 'It's hard. We know we're asking a lot of you.' -- Nurse coordinator at an adult CF care center
Share Your Stories
We invite you to share your stories or brief moments of care encounters -- good and bad -- so your insight can be used to promote a dialogue and exchange perspectives surrounding partnerships for sustaining daily care.
These stories will be used to identify strategies, conversation styles, and tips to share with care teams, adults with CF, and their families so that they can apply the Partnerships for Sustaining Daily Care (PSDC) concepts into their regular clinical practice and daily care routines.
So after you read this, take the time to self-reflect. Draw on your own experiences where you've had conversations (good or bad). Send us an email and share your story or ideas about sustaining daily CF care. We're listening at PSDCteam@cff.org.