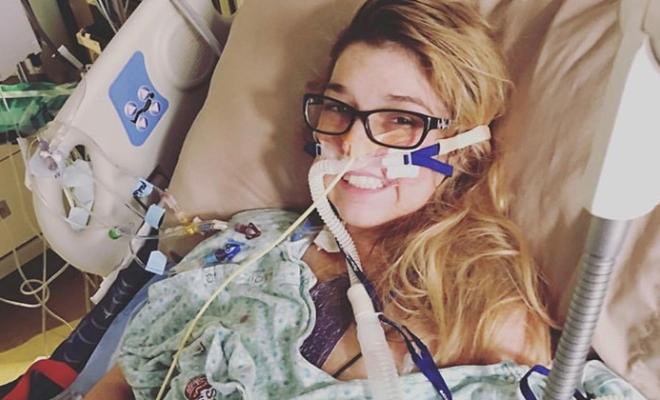
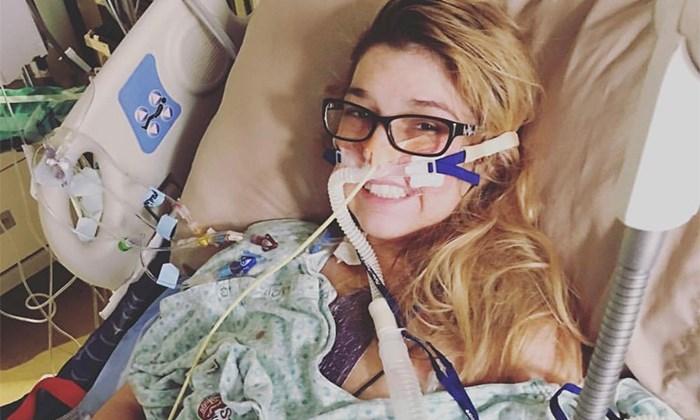
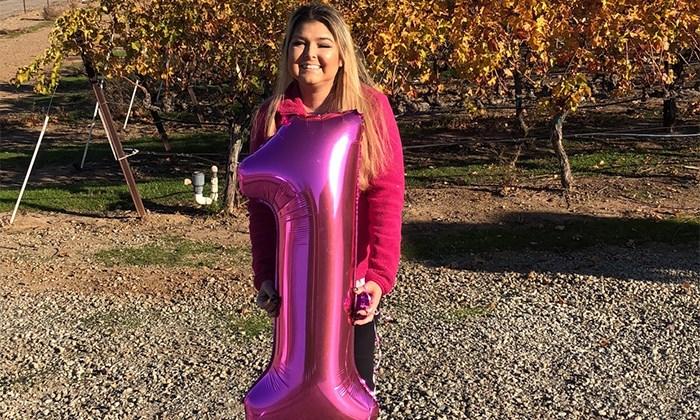On Nov. 30, 2016, I received a double-lung transplant from my selfless donor. The past year has been rough, but exciting and full of huge changes. I used to be on an oxygen leash 24/7, nebulized breathing treatments every four hours, and IV antibiotics every three weeks. Now, I am IV-less, rarely cough, and no longer use supplemental oxygen.
My journey started when, at the age of 23, I was unable to get my lung function above 30 percent FEV1. I was told that I needed to be evaluated for transplant. I was devastated and by myself at this clinic appointment. I couldn't believe that I was being told this was my last resort and that my CF was at end stage. I didn't want to come to terms with it, but I finally gave in and did all the necessary testing. On March 12, 2014, at the age of 24, I was put on the double-lung transplant list. I waited a long 973 days, almost two years and eight months, before I got the call.
I went into the transplant center on Nov. 29 (it happened to be Giving Tuesday) with all my family and friends there to celebrate that “we” finally got the call. My friends and family always say that “we” have CF because they feel it emotionally rather than physically. I rolled into the operating room about 30 hours after I received the call. On Nov. 30 at 6 a.m., I was told the lungs were a “go” and I was going to breathe. The surgery was a successful seven hours and 30 minutes.
We were told that my donor had been in a car accident and that the lungs had a couple of punctures in them, but that they were too good to pass up. Those punctures were patched up, scanned, and looked over thoroughly before they were put into my body. Because of this, my recovery was a bit lengthier than it is for most. I had to be re-intubated because my heart wasn't able to handle the stress of breathing on my own. I needed more assistance, which is pretty common right after transplant. They put too big of a tube in, which made my left vocal cord lazy and made it unsafe to swallow for my new lungs. I had to get a nasogastric (NG) tube put in, then they placed a gastro-jejunal (GJ) tube after.
I finally was able to eat real food on day 20. I had chest tubes in for about 30 days until the lung punctures were healed enough and not leaking air. I had a rough time adjusting to the high doses of medications and anxiety was taking over. Thankfully, I was able to get used to those medications. I walked without oxygen and did physical therapy every day. I got through those rough 32 days and moved to the apartment next to the hospital on New Year's Eve, where I had post-transplant clinic every other day for the next few weeks.
Finally, I was able to go home to my kitty and house on Valentine's Day. When I went home, I started pulmonary rehab to help strengthen my lungs and all my muscles. I had experienced atrophy of all my muscles while waiting for the transplant, so I have been working to get them all back. However, a few weeks after returning home, I had a routine X-ray and the doctors discovered I had a pneumothorax, a collapsed lung. My left lung had collapsed, and I had no idea because I was so used to not being able to breathe. I went to the ER and was admitted. Twenty days, another five-hour surgery, and two chest tubes later, I was breathing easy and able to go about my life.
After this whole crazy incident, I started my life again. I went on a hot air balloon ride, went to my first NBA game (a Warriors playoff game), walked the entire Great Strides walk in San Francisco, turned 28 years old, went to Disneyland, and was able to be in my best friend's wedding. Those all have been such amazing moments in my life since transplant, but the best celebration has to be my first “lung-iversary.” My best friends, Kelsey, Callie, Kim, and I went to see my favorite person on Earth, aka Taylor Swift, perform. We had shirts that read, “It's my first lung-iversary” and “Tiff's lung-iversary squad.” On the back it said my hashtag, “Reputation: #TIFFGOTLUNGS.” It was the best night. I had so many people come up and say how happy they were for me and in the process, I was able to raise awareness about CF and organ donation.
The celebration did not end there. A week later, my family and friends threw me a surprise lung-iversary party at our local winery. It was amazing, the place was decked out in pink, Taylor Swift lyrics, Minnie Mouse, my favorite Italian food, and a big pink “1” balloon. It was funny because people were asking, “where's the 1-year-old?” We couldn't help but laugh and tell them about my journey. This was such an amazing surprise and I couldn't help but thank my selfless donor. We said cheers to them and their family and hope that one day we will be able to thank their family in person. I wouldn't be alive had it not been for them checking that box on their license or signing up online. I am eternally grateful for this gift of life and I am happy to say I am breathing easy.