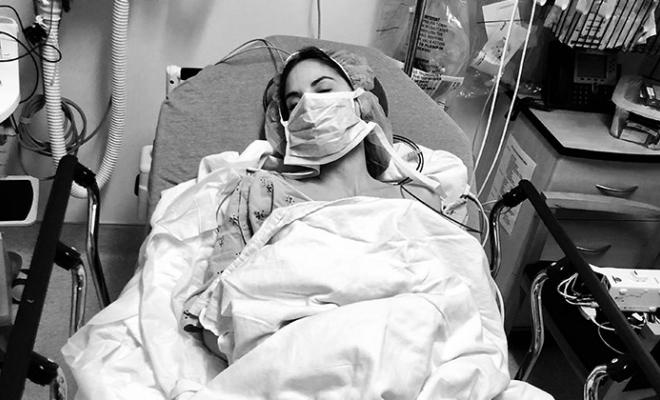
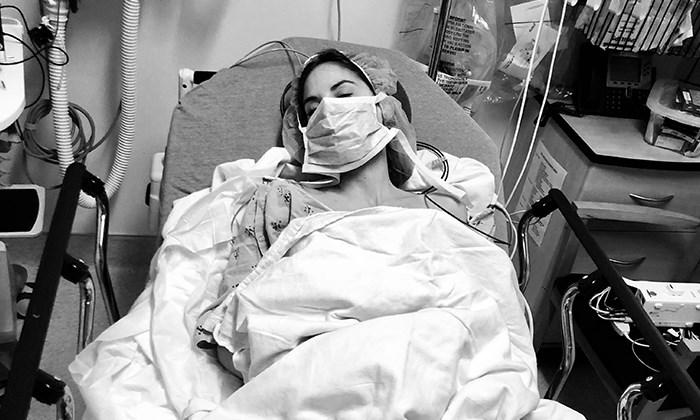
Lung transplant. Two words people with cystic fibrosis often hear throughout their medical care. At first, it's this idea, one that's far in the distance, something overwhelmingly large that doesn't really pertain to you. At least, not at the time. I couldn't relate when it was first mentioned to me, so I pushed it to the far corners of my mind, only revisiting the idea when I sympathized with my fellow CF warriors who were facing a transplant.
When I was told that I would definitely require a transplant in the future, I wasn't at a CF care center that best suited me so my first reaction was to decline. I knew what this meant in the big picture and it devastated me, but I never wanted to put my family through a transplant I didn't believe in.
I moved to Southern California when I was 32 years old and was hospitalized shortly after with an exacerbation. During that admission, I met my current doctor, who -- without a doubt -- changed and saved my life. I had never had a CF doctor like her before, and not only did I feel like she truly cared, but I finally had a doctor who listened to me. She treated me like an individual, not just a CF statistic. For the first time in more than a decade, I trusted the doctor fighting this battle with me, and the idea of getting a transplant one day became something that I absolutely wanted.
Cystic fibrosis is a progressive disease, and what I once couldn't relate to whatsoever -- lung transplant -- has now become the reality I face. My lungs are dying, and they are taking me along with them.
As I have gone through the transplant evaluation, there are things I want people to understand about what a transplant means. It is an involved process, and there are no answers or decisions made right away.
The transplant evaluation is a process that involves days of back-to-back procedures, from blood draws to ultrasounds, and days of appointments meeting with the transplant surgeon to psychiatrists to dietitians, all discussing your case and preparing it to be reviewed by the transplant committee -- the committee that decides if you are approved or not. Waiting for my results was mentally challenging, and I cried tears of joy and relief when I was told I was accepted.
I realized that once a person is listed for transplant, the call for new lungs could come at any time, so there are certain requirements that need to be met, such as staying within a four-hour distance of the transplant center and having the phone on at all times.
From blood type to size, the new lungs have to be an absolute perfect match. You receive a lung allocation score to determine where you are placed on the United Network for Organ Sharing (UNOS) waiting list. This score is usually a good indicator of how long you will wait until there is a match, which could be months or even years. Sadly, sometimes people don't live long enough for their transplant to take place. Organ donation is based on a scoring system, and there is an ethical debate about whether this system is completely fair. To a person on the transplant waiting list who sees donor lungs given to a seemingly healthier person, this can be a harsh reality.
It is difficult to determine when is the best time to list for transplant. It is a rollercoaster of emotions, and I've had to learn to hold on and go with the ride. The thought is, you need to be sick enough to need a transplant, yet strong enough to survive it.
Life after transplant doesn't mean you no longer have CF, although you will not have hours of breathing treatments. My CF medications will be replaced by a lifetime of immunosuppressants, which are vital to minimize the risk of organ rejection. I will have a new disease altogether, so to speak. Transplant gives the hope of many more years, but it does not take away the disease.
While many transplant statistics and survival rates are promising and encouraging, it is still the biggest type of surgery with the most risks one could undergo. I'm sometimes at a loss for words when I'm congratulated for getting listed, as a broad spectrum of emotions runs wild inside my mind. I am forever grateful for being approved and am optimistic for the day I get a new, healthy pair of lungs, but my road leading to that point is far from congratulatory.
For many years, my son has looked at me with a sparkle in his eye whenever he blows out a birthday candle or an eyelash from the palm of his hand. He smiles and says his only wish is for his mom to get new lungs. Every day I hope his wish comes true.
Join the conversation on Facebook.