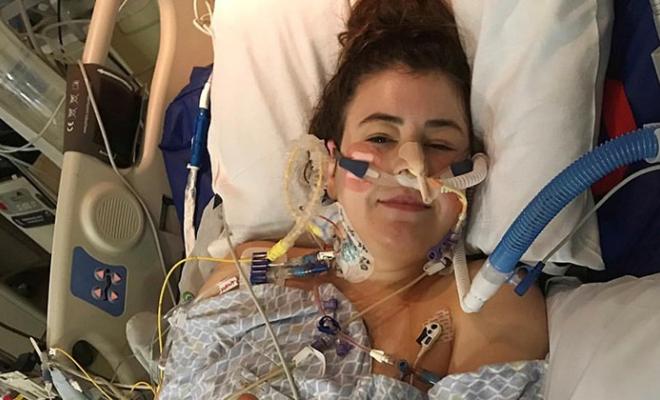
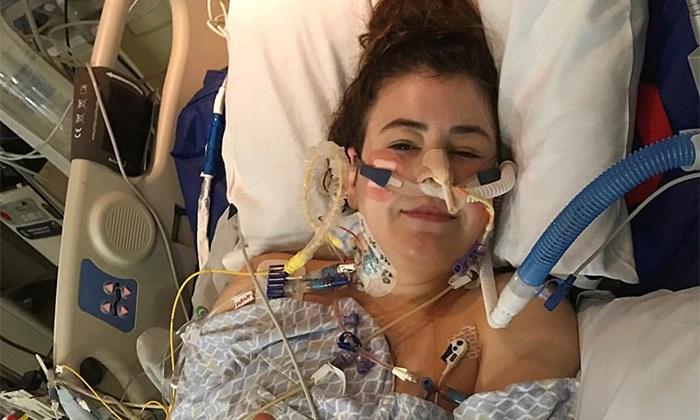
In September of 2018, I was starting a new chapter in my life with cystic fibrosis. I was in advanced stage lung disease, on supplemental oxygen 24/7, and managing my mental health. To say it was a difficult time is an understatement. I had no idea, though, that within a few months I would be told by my doctors that they were referring me to be evaluated for a double lung transplant.
I always knew transplant was going to be a part of my future; it was the reason my family and I moved from Kansas to the San Francisco Bay Area. But, no matter how much you prepare, or know what will be coming around the bend, it still hits you like a ton of bricks when you're told without a lung transplant your chance of survival is slim to nonexistent. At 27, I was seeing my friends and peers starting their careers, getting married, and having children and I was just trying to survive.
Going through the transplant evaluation was physically, mentally, and emotionally exhausting. The evaluation consisted of: chest X-rays; CT scans of my lungs, sinuses, and digestive system; endless amounts of bloodwork; an esophagram; SNIFF test; a right-heart catheter procedure; and meeting with a psychiatrist, social worker, the transplant team of doctors, nurse practitioners, and nurse coordinators. Thankfully, I already knew some of the doctors and nurse practitioners on the transplant team because they are also part of my cystic fibrosis care team. It was comforting to see familiar faces in very unfamiliar territory.
By the end of the four-day evaluation, I was depleted and hoped that the transplant team would tell me I was a good candidate for transplantation. I was shocked when they told me I wasn't a good candidate because I was considered “too healthy” to be listed for transplant. What was even crazier was that they were admitting me to the hospital for IV antibiotics because my lung function had dropped.
I was so confused, angry, scared, and tired. I was being told that I was “too healthy” to be listed for transplant, yet I was being admitted to the hospital because I had gotten sicker. I felt as if I was in a dream and just waiting to wake up.
Over the next five months I was deferred for transplant two more times even though I was in end-stage lung disease. I felt as if I was on a train platform waiting for the next train to come but I didn't know when -- or even if -- it would arrive. I was in limbo with no way to get out. It's strange when you're hoping to get sicker so you can ultimately get better.
On December 6, 2018, I was finally in “the window” to be listed for a lung transplant and placed on the United Network for Organ Sharing. When my nurse coordinator called to tell me the news I cried; I was in disbelief. I went through every emotion - excitement, fear, and sadness for my future donor and their family. It hit me full force right then that -- for my life to be saved -- someone else's life would be ending.
Less than 60 days later, while taking a nap, I got the call. At first, I was going to send it straight to voicemail because I was so exhausted, but something told me I needed to answer. On the other end of the line I hear, “We've got the perfect pair of lungs for you. How soon can you get the hospital?” I froze. I didn't know how to respond and in my typical fashion, I laughed and said, “Are you serious?” I wonder if the surgeon had ever heard that kind of response before? After accepting the lungs over the phone, I was scrambling around my apartment trying to figure out what to pack while simultaneously calling my parents, my siblings, and my best friend. I hadn't prepared! I thought I had all this time to figure out what I would pack. I also had wanted to write letters to those closest to me in case I didn't make it.
When I arrived at the hospital, one of the surgeons told me that this would probably be a “dry run” and there was only a 20 percent chance that the surgery would actually happen because my donor was still on life support. For the next seven hours, I waited, slept, and waited some more. It was around midnight that I told my parents I didn't think it was going to happen and that we should go drown our sorrows in pancakes at IHOP when they sent us home from the hospital. It was around 2 am when my nurse came in and announced that surgery was set for 6 am. I looked over at my mom and said, “Well, I guess we aren't going to IHOP anymore.” A few hours later I sent my goodbye texts to my siblings, hugged my parents, and was wheeled back to the operating room.
More than 10 hours later, I woke up in the ICU to the voices of my parents, my siblings (who had flown in from New York City and Baghdad), and my best friend. I was intubated, had six chest tubes, and was hooked up to endless antibiotics, fluids, and monitors. I was in an immense amount of pain, but I could breathe. It was such a strange sensation to take a breath and not immediately start coughing or feel as if I was suffocating.
February 1, 2019, my life was saved by my donor and their beautiful and selfless gift. When I wake up in the morning, I can feel my breath go all the way down to my toes. I send up a silent prayer to my hero, my donor. I can now live a life I only dreamed of having. I want to go back to school, start a career, and live independently. I'm able now to be a better daughter, sister, and friend to those I love. I even decided to start training for the New York City Half Marathon in 2020 with my sister! I keep my donor and their family in my heart every day and will do everything in my power to honor and make them proud.