I always knew I wanted to have children. So when I finally met my husband in my final year of graduate school at the age of 26, we did not wait long after we were married to start a family. We both understood the impact that cystic fibrosis can have on the reproductive system and accepted infertility as a very real possibility. We worked closely with my CF care team -- sorting through my medications to ensure that they were all “pregnancy-approved,” getting x-rays done in advance and making sure my PFTs were stable and I was healthy.
To our surprise, we got pregnant within three months. Other than a diagnosis of gestational diabetes (which is very common in pregnant women with CF), I had little to no issues throughout my pregnancy. In fact, my lung function increased during my last trimester! My CF doctor referred me to the high-risk obstetrician (OB) practice in the same medical system and hospital as my care team. It was incredibly comforting to know that if there were any issues during pregnancy, labor, delivery or recovery, I could easily reach out to my CF team and receive a quick response.
On Jan. 25, 2016, I delivered a beautiful baby boy named Jonah. My induced labor and delivery were incredibly successful, and as soon as Jonah was born I was immediately handed my nebulizers and any other medications I had missed during labor.
However, looking back on my time spent in the hospital for labor, delivery and recovery, I now understand the importance of planning and asking questions in preparation for giving birth. Women with CF are a rarity in the labor, delivery and recovery units, so advocating on my own behalf became incredibly important to my post-labor recovery and care. With much of my attention focused on my newborn son, taking care of myself became secondary to my son's health and well-being. But how could I be a good mother if I was not monitoring my own health?
Although I had spent time in the hospital's inpatient CF pulmonary unit in the past, this experience gave me new insight on dealing with nursing and medical staff who may not be specifically trained in CF. Here are some of my tips for women with CF planning their own pregnancy, labor and delivery:
1. Go on the hospital tour (even if it is your CF hospital) and ask a LOT of questions! I thought I asked questions, but looking back there were so many more I should have asked, like these:
- What medications will be available for me during my stay? (Medications like Cayston® may not be provided by the hospital.)
- Of the medications that are not provided, how can I obtain clearance to have them with me in the delivery and recovery unit?
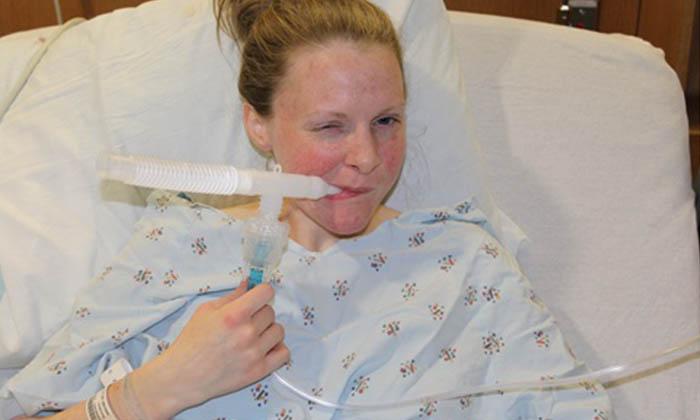
- What airway clearance technique is recommended after delivery, and what devices will be available for me to use during my hospital stay? (I typically use the Vest, but it was not accessible in the recovery unit at the hospital, so I ended up using the Aerobeka during my hospital stay. This turned out to be beneficial for me, as I needed a short break from the Vest during the healing process.
- Is there a person (i.e., charge nurse, nurse manager, unit manager, etc.) whom I can easily contact during my stay if I'm having difficulty communicating with the nursing staff?
- Can my enzymes be left in my room during my recovery? (I often had to wait up to an hour to get my enzymes to eat any meals or snacks. Post-labor and delivery is not a time you want to have to wait to get medications -- or food!)
2. Maintain good communication with your OB and CF care teams throughout your pregnancy, and request that they talk to each other, if necessary. When I was diagnosed with gestational diabetes, I occasionally felt like the “middleman” between my CF doctor and my OB in managing how to treat it. I had to be firm with my doctors and request that they discuss the details together before they offered me their suggestions and recommendations.
3. If you deliver at the hospital associated with your CF clinic, find comfort in knowing that your team is nearby if there are any complications.
4. Trust that the doctors and nurses (though they may not be experts on CF) want what is best for you and your baby.
My husband and I could not be more thrilled to be on this new, exciting journey with our healthy (and CF-free) little boy! The old adage of Henry Ward Beecher is true: “We never know the love of a parent till we become parents ourselves.”