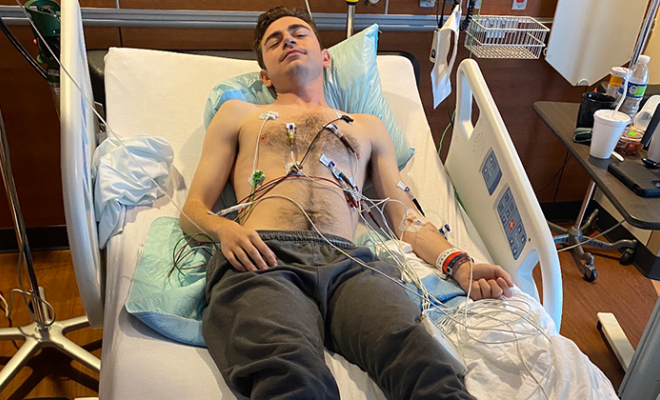
My journey all started with back pain. I was 26 and went to the gym every day, so I chalked the pain up to working out. But, I tried heating and icing and still there was no relief. I ignored it. One night I woke up and knew I had to throw up, but the pain was so severe I couldn’t walk to the bathroom. So, I army crawled to the bathroom and threw up blood and then called 911. When I got to the hospital, I was in so much pain that even morphine couldn’t take it away. The doctor came in and told me I had pancreatitis. I looked up — terrified.
Today, they screen all newborns for cystic fibrosis. Growing up, I was always sick. My immune system couldn’t fight anything off and I never knew why. Once I had my first bout of pancreatitis, it happened again every month for three years after that. My local hospital kept insisting it was pancreatitis, but I knew it wasn’t. That diagnosis didn’t make sense given my age and lifestyle.
I changed my lifestyle to fit what the hospital suggested, but it made no difference. I kept telling my doctors, “This doesn’t make sense.” But they ignored me and put me on pain meds and a nothing by mouth (NPO) diet for a week and sent me on my way to wait for it to happen again. That is, until during one flare-up, my lipase levels were so high that my local hospital said they couldn’t help me, so they put me in an ambulance to Beth Israel Deaconess in Boston.
Once there, I met a doctor who truly saved my life. He looked at all the tests that other doctors had tried and ran them again himself. My MRI showed an extremely scarred pancreas due to the swelling it had endured over the last 36 months. He thought outside of the box and said, “We’re going to have you take a sweat test to test you for cystic fibrosis.” It came back positive for the F508del mutation.
While the diagnosis was scary, I finally had a definitive answer as to why the majority of my last 36 months was spent in the hospital, or worrying about when another pancreatic flare would land me back in the hospital.
At Beth Israel, I was fitted with a nasogastric feeding tube, which is a tube that went up my nose down my esophagus, bypassing my pancreas and connecting to my stomach. The idea was to give my pancreas a break during digestion. I had special formula fed through the tube and couldn’t eat or drink otherwise. The tube hung next to my bed when I slept, and then it went in a backpack when I was out in public. The stares I got when having a tube taped to my face were difficult at first, but I had to remind myself that this was saving my life and I got to be out with friends and family instead of stuck in a hospital.
Cystic fibrosis commonly presents in the lungs before the pancreas, but I am a rare case where it happened the opposite way. I now manage my pancreas with the enzymes that most CF patients take. While I am fortunate to be living a fairly normal life right now, CF still affects me daily. I have to be sure that I have medication on me everywhere I go, and any new twinge or pain puts me into immediate fear. I have to be careful who I surround myself with because of the “6 feet apart rule.” I work in a hospital and have to avoid an entire unit because a patient there also has CF and we would put each other in life threatening danger. I have also noticed I run out of breath more quickly than I did in the past; and I know CF is going to severely affect my lungs eventually.
I am extremely grateful that I was diagnosed and hope that cystic fibrosis continues to be at the forefront of medical innovation. The more we learn, the longer the lifespan is for someone living with CF. I talk about it as much as I can just to bring awareness to people that, sometimes, you have to advocate for yourself. It may not be a rare case like mine, or it may be even rarer, but you know your body best. I knew my body had a different explanation and I finally found a doctor who listened to me.
Interested in sharing your story? The CF Community Blog wants to hear from you.